Functional and Psychosocial Optimization in Below-Knee Amputation for Persistent Refractory Diabetic Foot Osteomyelitis: A Unique Case Report of Autologous Tissue Reconstruction with Symbolic Skin Preservation and Literature Review
Abshiro H Mayow1,*, Shirice Lesane1, Abdi Mayow2 and Frederick Tiesenga3
1St George’s University School of Medicine, Grenada
2St. Cloud Technical and Community College, St Cloud, MN, USA
3Department of Surgery, Community First Medical Center, Chicago, IL, USA
Received Date: 06/07/2025; Published Date: 06/08/2025
*Corresponding author: Abshiro H Mayow, St George’s University School of Medicine, Grenada
Abstract
Diabetes mellitus remains a major global health challenge, a global public health burden affecting over 463 million adults, frequently leading to complications such as neuropathy, nephropathy, and retinopathy. Among these, diabetic foot ulcers stand out due to their strong association with chronic infection, critical limb ischemia, and a high incidence of non-traumatic lower extremity amputations. DFUs often arise from a combination of peripheral neuropathy, vascular insufficiency, and impaired immune function. Poor glycemic control further heightens the risk, creating a chronic inflammatory environment that is prone to infection and delayed wound healing. Osteomyelitis is a frequent and severe complication in patients with recurrent DFUs. It is commonly caused by polymicrobial pathogens, most notably Staphylococcus aureus and Pseudomonas aeruginosa. When such infections are unresponsive to medical management—including debridement, antibiotics, and advanced wound care—surgical intervention such as below-knee amputation (BKA) becomes imperative to prevent systemic infection, sepsis, and death.
We present the case of a 55-year-old male with persistent, recurrent diabetic foot osteomyelitis due to poorly controlled type 2 diabetes, unresponsive to extensive non-surgical management. Ultimately, the patient underwent a BKA incorporating an innovative, patient-centered approach: preservation of a healthy, tattooed skin area for autologous coverage of the surgical site. This technique promoted functional recovery and contributed positively to the patient's psychological well-being. This case highlights the importance of making timely surgical decisions and integrating psychosocial factors in managing complex diabetic foot infections.
Introduction
Diabetic Foot Ulcers (DFUs) are among the most debilitating complications of diabetes mellitus, affecting nearly one in four diabetic patients during their lifetime and accounting for over two-thirds of all non-traumatic lower extremity amputations globally [1,2]. These chronic wounds typically result from a combination of peripheral neuropathy, microvascular insufficiency, and impaired immune response, disrupting wound healing and increasing vulnerability to infection [2]. Persistent hyperglycemia contributes to endothelial dysfunction and impairs leukocyte function, thereby reducing tissue oxygenation and phagocytic efficiency, which facilitates bacterial invasion and biofilm formation in chronic wounds. Diabetic Foot Osteomyelitis (DFO), a progressive infection of bone arising from the contiguous spread of a foot ulcer, develops in approximately 20% of DFUs and drastically increases the risk of limb loss if inadequately treated [3]. In DFO, addressing risk factors for re-infection, such as poor blood supply, impaired wound healing, and comorbid conditions, is crucial, as these factors contribute to chronic infections and increase the likelihood of complications, including prolonged antibiotic therapy and amputation. Considering these factors is essential for improving the management and outcomes of diabetic foot osteomyelitis [4]. DFO remains diagnostically elusive, despite its prevalence, due to overlapping signs with soft tissue infections and nonspecific clinical presentations. These emphasize the urgent need for improved diagnostic strategies and early intervention to prevent irreversible outcomes such as multi-organ failure and death.
From a microbiological standpoint, DFO is often polymicrobial, with Staphylococcus aureus and Pseudomonas aeruginosa forming persistent biofilms that shield pathogens from immune clearance and limit the efficacy of antibiotic therapy [5]. The diabetic metabolic environment, marked by chronic hyperglycemia, alters host-microbe dynamics by impairing neutrophil chemotaxis, cytokine signaling, and glycemic homeostasis. This complex interplay between endocrine dysfunction and microbial colonization underpins the chronicity of DFO and its resistance to treatment. Accurate diagnosis typically relies on bone biopsy, deep tissue cultures, and MRI imaging; however, delays in recognition or inadequate sampling can lead to treatment failure [6]. Clinicians must also consider systemic factors, such as serum hemoglobin A1c levels, glycated hemoglobin (HbA1c), nutritional deficiencies, and concurrent vascular disease, which significantly influence infection resolution and surgical candidacy [2, 7].
Standard treatment for DFO begins with prolonged systemic antibiotics, surgical debridement, and relieving pressure from the affected foot using specialized footwear or mobility aids, a process known as offloading, which requires extended monitoring over weeks or months [8]. However, persistent infection, poor glycemic control, patient non-compliance, and structural deformities frequently limit the success of conservative care [3,9]. When osteolysis, necrosis, or systemic involvement is present, Below-Knee Amputation (BKA) becomes not only appropriate but often life-saving to prevent sepsis and multiorgan failure [10,11]. Although amputation is typically reserved as a last resort, timely surgical intervention, integrated with multidisciplinary planning, has been shown to preserve function and enhance outcomes [12]. Despite this, literature rarely addresses the psychosocial burden of amputation or the role of body image preservation in recovery. Humanistic approaches, such as intentionally preserving culturally or personally significant skin, like tattoos, may provide psychological benefits and support holistic recovery [13,14].
This is a rare and compelling case report involving a 55-year-old man with uncontrolled type 2 diabetes who developed chronic, recurrent osteomyelitis involving both the foot and proximal tibia. After multiple failed conservative management, including debridements, IV antibiotics, and wound care, he underwent a BKA. This case is distinct due to the intentional intraoperative preservation of a tattooed skin area with symbolic value, which was used as autologous coverage for the amputation site. This novel approach minimized complications while honoring the patient’s identity and emotional needs. It emphasizes the importance of humanistic and patient-centered strategies in surgical decision-making. It underscores the need for personalized care models that address both clinical outcomes and the psychosocial dimensions of recovery.
Case Presentation
A 55-year-old White male with a five-year history of poorly controlled type 2 diabetes mellitus presented to the emergency department with worsening pain, purulent drainage, and a foul odor from a chronic right lower extremity wound. His past medical history was significant for recurrent diabetic foot osteomyelitis, for which he had undergone four previous surgical procedures on the same limb, including irrigation and debridement, placement of antibiotic beads, and insertion of an antibiotic-impregnated spacer into the proximal tibia. He had a longstanding history of poor glycemic control (HbA1c >10%) and admitted to daily cigarette smoking and nonadherence to his daily oral anti-diabetic medications of metformin and glimepiride.
Upon examination, the patient appeared pale and dehydrated, with a pulse of 106 beats per minute, blood pressure of 164/80 mmHg, and an oxygen saturation of 95%. Local Examination findings included peripheral edema and tenderness. An ulcer was noted on the plantar surface of the right foot, with a fibrinous base and surrounding maceration (Figure 1a–b). Additional examination on the surrounding area revealed a separate chronic 5 × 3 cm ulcer with fibrinous exudate on the anterior proximal tibia with exposed spacer portions (Figure 2). Laboratory data showed leukocytosis (WBC 14.2 × 10^9/L), elevated C-reactive protein (CRP) (96 mg/L), anemia (Hb 11 g/dL), and thrombocytopenia (platelets 340 × 10^9/L). Imaging (Figure 3) indicated cortical thickening, focal osteolysis, and periosteal reaction consistent with chronic osteomyelitis. MRI also showed edema and signal changes in the tibialis posterior muscle, confirming the diagnosis. Consistent with prior cultures, deep tissue samples revealed polymicrobial infection, including Staphylococcus aureus and Pseudomonas aeruginosa.
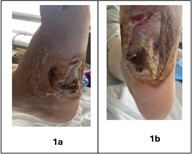
Figure 1(a-b–): Gross clinical photographs of a chronic diabetic ulcer on the plantar surface of the right foot. Figure 1a shows a direct plantar view displaying ulceration with a fibrinous base and surrounding tissue maceration. Figure 1b demonstrates the Oblique plantar view, highlighting the lesion's depth, borders, and peripheral inflammation.
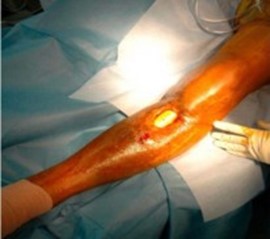
Figure 2: Gross image of the anterior aspect of the right proximal tibia showing a 5 × 3 cm wound with exposed soft tissue, fibrinous exudate, and partial exposure of the underlying antibiotic spacer.
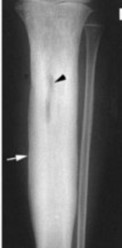
Figure 3: An X-ray of the right lower extremity demonstrates features consistent with chronic osteomyelitis (Black arrow), including cortical thickening (white arrow), periosteal new bone formation, focal sclerosis, and areas of bone destruction.
Outpatient management remained unsuccessful as the patient's hyperglycemia remained uncontrolled despite medication adjustments and dietary interventions, thus contributing to the progressive nature of the infection. Despite several weeks of intravenous antibiotics, infectious disease consultation, and culture sensitivity studies, the wound failed to improve and continued to exhibit purulent drainage. While in the hospital, anti-diabetes agents were discontinued, and hyperglycemia was managed with physiological insulin. Nutrition services initiated a diabetic-appropriate, low-glycemic index diet, eventually stabilizing glucose levels (<200 mg/dL) before surgery. Given the complexity and severity of the infection, the surgery team determined that the only viable curative option was a below-knee amputation (BKA). The patient was informed of the possibilities with full explanations given, and he chose to “proceed with surgery and do everything possible to save” his life. The patient demonstrated an understanding of his treatment regimen, which included multiple rounds of medical management, culture-directed intravenous antibiotics, and surgical debridements; however, the infection persisted. Due to treatment-refractory diabetic foot osteomyelitis and the risk of systemic spread, below-knee amputation (BKA) was ultimately required as a life- and limb-saving intervention. A humanistic approach gave special surgical consideration to preserving a region of healthy, tattooed skin proximal to the ulcer. The tattoo was culturally symbolic to the patient, and maintaining it offered an opportunity to address both reconstructive and psychosocial aspects of his care. During surgery, a portion of the healthy skin was successfully used as autologous coverage for the amputation site (Figures 4a and 4b).
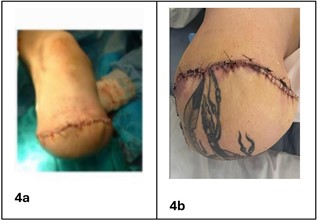
Figure 4(a-b–): Postoperative images following below-knee amputation with innovative reconstructive preservation. Figure 4a depicts a Clean surgical site on the right lower extremity showing well-approximated sutures and absence of drainage or erythema. Figure 4b shows Preservation of a tattooed region on healthy skin, which was utilized as autologous tissue coverage for the wound, serving both functional reconstruction and symbolic significance to the patient.
Postoperatively, the patient was managed with IV vancomycin and cefepime. His vitals remained stable, and wound healing proceeded without complication. Daily dressing changes revealed a clean surgical site with no signs of erythema, drainage, or dehiscence. Sensory function was preserved distal to the incision, and pain was managed effectively. Physical therapy was initiated within days, and by discharge, the patient was mobilized with a walker and was compliant with the recommended physical therapy, nutritional, and glycemic prescriptions. The patient had significant physical improvement at follow-up and expressed emotional satisfaction with the outcome. He noted that preserving his tattoo provided a sense of identity and continuity that aided his psychological adjustment post-amputation. The integration of functional and symbolic preservation played a crucial role in supporting the physical and emotional dimensions of his recovery. Overall, this case uniquely bridges surgical innovation with patient-centered values, demonstrating that successful outcomes in refractory diabetic foot osteomyelitis are defined not solely by infection control or limb salvage but also by preserving identity, dignity, and emotional resilience.
Discussion
Diabetic foot ulcers are one of the well-known complications of Diabetes Mellitus and hence impose significant morbidity, mortality, and healthcare costs globally [2]. These chronic wounds develop due to multiple factors, including peripheral neuropathy, vascular insufficiency, defective wound healing, persistent hyperglycemia, and systemic inflammation, leading to increased immune compromise and endothelial injury. Such cascading pathophysiological events create conditions for the progressive dysfunction of vascular and endothelial systems, as well as functional impairment of the neuropathic system [1,2]. Smoking exacerbates the pathophysiology of diabetic foot osteomyelitis by impairing microvascular circulation and compromising immune function, thereby impairing the body's ability to fight infection and delaying tissue healing, which accelerates the progression of the disease and complicates treatment [15]. These factors increase the patient's risk of ulcer formation and limit their effective healing environment, which is highly vulnerable to secondary infections, such as osteomyelitis [16]. Diabetic foot ulcers (DFUs) affect approximately 25% of individuals with diabetes, with infections complicating over two-thirds of cases and leading to a high risk of amputation [2, 17]. Key factors, such as peripheral neuropathy, vascular insufficiency, and chronic hyperglycemia, hinder healing and increase vulnerability to infection [1,9]. These ulcers create an environment conducive to bacterial colonization, requiring comprehensive care to prevent severe complications. The pathophysiology of diabetic foot osteomyelitis presents significant challenges in diagnosis and management; therefore, a better understanding of the complexities of this condition underscores the importance of early intervention and comprehensive care [1,5,9]. Consequently, special-case investigations are critical for prognosis, managing underlying conditions, optimizing patient outcomes, and preventing irreversible complications.
This report investigates a rare case of a 55-year-old white male patient with a chronic non-healing diabetic foot ulcer. The patient had recurrent osteomyelitis infections requiring several hospitalizations, consisting of multiple therapies including minor surgeries, wound care, as well as oral and systemic antibiotics. His condition had progressed due to persistent hyperglycemia and long-term tobacco use in addition to noncompliance with diabetes drugs, which led to osteomyelitis infections eroding through bone. Because the infection did not respond to treatment and could spread in the body, a below-knee amputation was seen as necessary to save his life. After the operation, the man showed noticeable improvement, with stable vital signs and a reduction in signs of inflammation. Postoperatively, the patient displayed remarkable clinical improvement, with vital signs stabilized, scant wound exudate, and decreased inflammatory markers. This rare case demonstrates the need to address the biological aspects of osteomyelitis, its psychological ramifications, and the need to retain patient identity through reconstructive procedures. It also highlights the urgency and multidisciplinary nature of the intervention addressing physical and mental health.
Osteomyelitis occurs in close pronearof patients with DFU or diabetic foot infectations, respectively; approximately 90% of those cases are found in the forefoot A reduced immune system and poor blood circulation could also be the reasons why uncontrolled diabetic patients suffer from osteomyelitis-the entry point, therefore, becomes from the skin to tissue to bone. Skin ulcer-to-bone transfer of bacteria usually occurs in diabetic foot osteomyelitis. Their activities cause chronic inflammation, entry of white blood cells, changes in blood flow, and death of bone tissue, further aggravating the symptomatology and treatment of DFUs [17]. Diabetic foot osteomyelitis is a complex and rapidly progressing complication of diabetes that requires immediate and effective intervention due to its potential for systemic spread. Patients typically present with signs of localized infection, including erythema, swelling, warmth, and purulent discharge, accompanied by radiological evidence confirming bone involvement [18]. In severe cases, such as this patient's, the ulcer can be massively open with signs of necrosis due to persistent infection. Initiating treatment is crucial for patients with osteomyelitis, in addition to robust glycemic control. As such, a standard regimen of conservative management is repeated debridement, irrigation, and a long course of broad-spectrum antibiotics. Emerging Scientific evidence suggests that short-course and oral antibiotics may offer viable alternatives to long-term hospitalization, improving patient compliance and reducing healthcare costs [8]. Unfortunately, these conservative approaches have limitations, with early surgical intervention being crucial to prevent progression to foot necrosis, sepsis, and multi-organ dysfunction. Poor glycemic control, non-compliance, and smoking severely hinder the success of conservative treatments, resulting in persistent infections and complications [11, 19]. All this evidence underscores the urgent need for a multispecialty and aggressive approach to diabetic foot osteomyelitis to prevent complications and improve patient outcomes.
The critical modifiable risk factors in our patients include persistent high blood sugar levels, non-compliance with diabetes medications, and smoking, which contribute to the ineffectiveness of these treatments, leading to osteomyelitis eroding through bone. Early surgical intervention, such as a below-knee amputation, was required to prevent life-threatening complications like sepsis and multi-organ dysfunction. Surgical and antibiotic treatment, as well as control, remain essential elements in the management of this condition [3,8]. Due to the complexities surrounding diagnosis and management in diabetic foot osteomyelitis, one must carefully unravel its underlying mechanisms and include the role of lifestyle factors such as smoking in making the condition more complex. The pathogenesis and mechanism of diabetic foot osteomyelitis are driven by a complex interplay of immune dysfunction, vascular insufficiency, and hyperglycemia, with smoking exacerbating these underlying mechanisms [18,19]. Smoking compounds these factors by further reducing blood flow and inhibiting immune response. Smoking induces vascular constriction and decreases oxygen delivery to tissues, exacerbating ischemia and impairing the body's ability to fight infections.
Furthermore, nicotine in tobacco exposure impairs neutrophil function, which reduces the body's ability to combat bacterial infections effectively [19]. In this case, the patient's smoking history significantly accelerated the progression of the proinflammatory nature of osteomyelitis by impairing circulation and weakening immune defenses, which allowed bacteria to migrate from the skin ulcer into the bone. Persistent chronic inflammation leads to impaired blood flow, resulting in subsequent tissue and bone necrosis, which further complicates the clinical situation [17]. These underlying mechanisms for diabetic foot osteomyelitis, such as immune impairment and microbial resistance, create a great need for individualized treatment. This is particularly crucial in immunocompromised patients like this patient with uncontrolled diabetes, where addressing modifiable risk factors is imperative to successfully managing the current condition and preventing infections. Although hyperglycemia, and smoking played a pivotal role in the progression of this patient's diabetic foot osteomyelitis by exacerbating poor circulation and impairing immune function, which contributed to the spread of infection from the skin ulcer to the bone, However, one crucial aspect is considering the psychological and emotional impacts of diabetic foot osteomyelitis, as it comes with significant amounts of suffering; much psychosocial support is needed to promote comprehensive rehabilitation and recovery [16,19].
Mental ailments such as depression and anxiety are highly prevalent in individuals with chronic diseases, exacerbating physical symptoms, impairing treatment adherence, and accelerating disease progression. Preserving aspects of self-identity, such as tattoos, has been shown to mitigate psychological distress, including anxiety and body dysmorphia, thereby promoting better mental health outcomes and improving overall quality of life [20,21]. The psychological well-being of patients with diabetic foot osteomyelitis is compromised mainly because this is a chronic condition, one that has severe implications, one of which can include loss of limb. We emphasize the importance of preserving the patient's symbolic identity, which can be achieved by integrating tattoos into reconstructive surgery. Such preservation has been shown to have a positive impact on mental health, improving body image and promoting psychological recovery [22]. Studies suggest that cultural identity and body image are critical to address in medical procedures for chronic conditions like diabetic foot osteomyelitis [8]. A multidisciplinary care approach and team-based interventions in the surgery field have been shown to improve patient outcomes and cost-effectiveness, emphasizing the value of collaborative care models in managing complex surgical cases [23]. As a result of the infection's severity and multiple risk factors, and by scientific recommendations, a multidisciplinary team (MDT) approach became crucial for addressing both the biological and psychosocial aspects of the treatment. Surgery, infectious diseases, and endocrinology experts improved patients’ outcomes through comprehensive care.
This case supports that Psychosocial care must be incorporated into clinical consideration to prevent anxiety and depression, as is often seen in many amputees, and reconstructive techniques should not solely aim for functional outcomes but also address psychological and emotional aspects, such as preserving tattoos [21, 24]. We strongly emphasize the importance of cultural awareness and respect for patients, which are crucial in providing exceptional, individualized, patient-centered care, as supported by scientific literature and our examination of this case. While the approach in this case offers promising insights into treating diabetic foot osteomyelitis, several limitations need to be addressed in future research. One limitation is the feasibility of tattoo preservation in every case, as its applicability may depend on patient preference, mental health status, and the clinical condition of the affected area [22]. Future research should focus on identifying specific variables contributing to re-infection after treatment for diabetic foot osteomyelitis, including microbial resistance patterns, glycemic control, immune response dysfunction, vascular insufficiency, smoking, and patient adherence to treatment protocols, to refine prevention and management strategies. Future research must focus on specific variables such as glycemic control, smoking status, vascular health, and microbial resistance, as these factors significantly influence the risk of re-infection in diabetic foot osteomyelitis. Current literature emphasizes the need to address these variables through targeted interventions and personalized care strategies to improve treatment outcomes and reduce the recurrence of infections [25,26].
Additionally, incorporating aesthetic preservation into diabetic foot osteomyelitis treatment is a relatively new concept, and further studies are needed to evaluate its long-term psychological benefits, particularly in terms of body image and cultural significance [26,27]. Current studies suggest that early and aggressive interventions significantly improve outcomes. However, this area requires further targeted research on patient-care models, clinical trials, and genetic profiling to enhance the precision of prevention and treatment strategies [26]. According to emerging scientific evidence,short-course and oral antibiotics could provide alternatives to long-term hospitalization and improve patient compliance [8,18]. It is crucial for future research to explore various variables and options while addressing the psychosocial aspects of care to ensure the development of holistic treatment strategies. This case highlights the need for a multidisciplinary approach that incorporates both functional and psychosocial factors in managing diabetic foot osteomyelitis, ultimately improving patient outcomes [11,12]. Humanistic interventions, such as tattoo preservation, pave the way for a more resilient path toward achieving optimal treatment outcomes and aiding patients' psychological recovery [13,14]. Hence, a comprehensive and compassionate approach, integrating medical and psychosocial care, is crucial to improve patient outcomes and quality of life in managing diabetic foot osteomyelitis.
Conclusion
Overall, this case report is a crucial addition to the literature on diabetic foot osteomyelitis, highlighting the significant challenges in managing this condition, particularly in patients with poorly controlled diabetes and multiple risk factors. The rapid progression of infection despite initial conservative treatments underscores the need for timely, aggressive surgical intervention, such as below-knee amputation, to prevent further complications like systemic infection and multi-organ failure. Importantly, this case highlights the importance of individualized approaches, such as incorporating tattoo preservation during surgery, in enhancing the patient's psychosocial well-being. This approach reduces postoperative complications and preserves the patient's identity, positively influencing mental health and recovery. For example, Early and aggressive intervention for diabetic foot osteomyelitis, alongside managing glycemic control and addressing risk factors, remains critical for improving outcomes. However, including aesthetic preservation in surgical management is crucial and remains underexplored. The key lesson for clinicians is the need for a comprehensive, multidisciplinary approach that combines humanistic, physical, and psychosocial considerations. Future studies should investigate the long-term psychological effects of aesthetic preservation and explore personalized treatment strategies for diabetic foot osteomyelitis to improve clinical outcomes further. This case requires a comprehensive approach to diabetic foot osteomyelitis, where surgical, psychological, and personalized interventions collaborate to optimize patient care outcomes.
References
- Akkus G, Sert Diabetic foot ulcers: A devastating complication of diabetes mellitus continues non-stop despite new medical treatment modalities. World journal of diabetes, 2022; 13(12): 1106–1121. https://doi.org/10.4239/wjd.v13.i12.1106.
- Katherine McDermott, Michael Fang, Andrew JM Boulton, Elizabeth Selvin, Caitlin W Hicks. Etiology, Epidemiology, and Disparities in the Burden of Diabetic Foot Ulcers. Diabetes Care, 2023; 46(1): 209–221. https://doi.org/10.2337/dci22-0043.
- Lázaro Martínez JL, García Álvarez Y, Tardáguila-García A, García Morales E. Optimal Management of Diabetic Foot Osteomyelitis: Challenges and Solutions. Diabetes, metabolic syndrome and obesity: targets and therapy, 2019; 12: 947–959. https://doi.org/10.2147/DMSO.S181198.
- Zhang K. Further considerations on risk factors for re-infection in diabetic foot osteomyelitis: Insights and recommendations for future research. Wound Repair and Regeneration. Advance online publication, 2023. https://doi.org/10.1111/wrr.70022.
- Johani K, Fritz BG, Bjarnsholt T, Lipsky BA, Jensen SO, Yang M, et al. Understanding the microbiome of diabetic foot osteomyelitis: insights from molecular and microscopic approaches. Clinical microbiology and infection: the official publication of the European Society of Clinical Microbiology and Infectious Diseases, 2019; 25(3): 332–339. https://doi.org/10.1016/j.cmi.2018.04.036.
- Coşkun B, Ayhan M, Ulusoy S. Relationship between Prognostic Nutritional Index and Amputation in Patients with Diabetic Foot Ulcer. Diagnostics (Basel, Switzerland), 2024; 14(7): https://doi.org/10.3390/diagnostics14070738.
- Castellino LM, Crisologo PA, Chhabra A, Öz OK. Diabetic Foot Infectious disease clinics of North America, 2025; S0891-5520(25)00019-4. https://doi.org/10.1016/j.idc.2025.02.014.
- Gachet B, Schechter MC, Armstrong DG, Robineau O, Senneville Not All in Vain: Oral Antibiotics for Diabetic Foot Osteomyelitis: A Narrative Review. Journal of Clinical Medicine, 2025; 14(5): 1405. https://doi.org/10.3390/jcm14051405.
- Lauri C, Leone A, Cavallini M, Signore A, Giurato L, Uccioli L. Diabetic Foot Infections: The Diagnostic Challenges. Journal of Clinical Medicine, 2020; 9(6): 1779. https://doi.org/10.3390/jcm9061779.
- Aragón-Sánchez J, Víquez-Molina G, Rojas-Bonilla JM. Polymicrobial infection in bone biopsies and relapse in diabetic foot osteomyelitis: The role of soft tissue involvement. Wound Repair and Regeneration, 2025; 33(1): e13246. https://doi.org/10.1111/wrr.70011.
- Maurer SM, Hepp ZS, McCallin S, Waibel FWA, Romero FC, Zorman Y, et al. Short and oral antimicrobial therapy for diabetic foot infection: a narrative review of current knowledge. Journal of bone and joint infection, 2022; 7(2): 61–70. https://doi.org/10.5194/jbji-7-61-2022.
- Taberna M, Gil Moncayo F, Jané-Salas E, Antonio M, Arribas L, Vilajosana E, et al. The Multidisciplinary Team (MDT) Approach and Quality of Care. Frontiers in oncology, 2020; 10: 85. https://doi.org/10.3389/fonc.2020.00085.
- Lee Roze des Ordons A, de Groot JM, Rosenal T, Viceer N, Nixon How clinicians integrate humanism in their clinical workplace-'Just trying to put myself in their human being shoes'. Perspectives on medical education, 2018; 7(5): 318–324. https://doi.org/10.1007/s40037-018-0455-4.
- Liao X, Li S, El Akkawi MM, Fu X, Liu H, Huang Y. Surgical amputation for patients with diabetic foot ulcers: A Chinese expert panel consensus treatment guide. Frontiers in Surgery, 2022; 9: 1003339. https://doi.org/10.3389/fsurg.2022.1003339.
- Klein LW. Pathophysiologic Mechanisms of Tobacco Smoke Producing Current cardiology reviews, 2022; 18(6): e110422203389. https://doi.org/10.2174/1573403X18666220411113112.
- AbdElrahman Elnour Eltilib A. Association Between Smoking and Foot Ulcer among Patients with Diabetes Mellitus, Wad Medani, Sudan Journal of Medical Sciences, 2021;16(4): 450-463. https://doi.org/10.18502/sjms.v16i4.9943.
- Giurato L, Meloni M, Izzo V, Uccioli L. Osteomyelitis in diabetic foot: A comprehensive overview. World journal of diabetes, 2017; 8(4): 135–142. https://doi.org/10.4239/wjd.v8.i4.135.
- Alkhalfan Y, Lewis TL, Kavarthapu V, Hester Investigation and management of diabetic foot osteomyelitis: An update for the foot and ankle orthopaedic surgeon. Journal of clinical orthopaedics and trauma, 2023; 48: 102330. https://doi.org/10.1016/j.jcot.2023.102330.
- Xia N, Morteza A, Yang F, Cao H, Wang Review of the role of cigarette smoking in diabetic foot. Journal of diabetes investigation, 2019; 10(2): 202–215. https://doi.org/10.1111/jdi.12952.
- Clarke DM, Currie KC. Depression, anxiety, and their relationship with chronic diseases: a review of the epidemiology, risk and treatment evidence. The Medical journal of Australia, 2009; 190(S7): S54–S60. https://doi.org/10.5694/j.1326-5377.2009.tb02471.x.
- McGloin H, Devane D, McIntosh CD, Winkley K, Gethin Psychological interventions for treating foot ulcers and preventing their recurrence, in people with diabetes. The Cochrane database of systematic reviews, 2021.
- Sraj S, Farley B, Turner A, Woodberry K. Managing and preserving tattoos during orthopaedic surgery. Journal of the American Academy of Orthopaedic Surgeons, 2025; 33(5): 221–230. https://doi.org/10.5435/JAAOS-D-24-00596.
- Davis MJ, Luu BC, Raj S, Abu-Ghname A, Buchanan Multidisciplinary care in surgery: Are team-based interventions cost-effective? The surgeon: journal of the Royal Colleges of Surgeons of Edinburgh and Ireland, 2021; 19(1): 49–60. https://doi.org/10.1016/j.surge.2020.02.005.
- Tenna S, Delle Femmine PF, Pendolino AL, Brunetti B, Persichetti Tattoo preservation during surgical procedures. Open Access Surgery, 2014; 7: 19–27. https://doi.org/10.2147/OAS.S36884.
- Lavery LA, Reyes MC, Najafi B, Coye TL, Sideman M, Siah MC, et al. The infected diabetic foot: Risk factors for re-infection after treatment for diabetic foot osteomyelitis. Wound Repair and Regeneration, 2025; 33(1): e13246. https://doi.org/10.1111/wrr.13246.
- Kumlien C, Acosta S, Björklund S, Lavant E, Lazer V, Engblom J, et al. Research priorities to prevent and treat diabetic foot ulcers—A digital James Lind Alliance Priority Setting Diabetic Medicine, 2022; 39(12): e14947. https://doi.org/10.1111/dme.14947.
- Ren J, Gao H, Luo W, Lu S, Fu C, Wang H, et al. Risk Factors, Microbiology, and Prognosis of Diabetic Foot Osteomyelitis: A Retrospective Cohort Study. Endocrine practice: official journal of the American College of Endocrinology and the American Association of Clinical Endocrinologists, 2025; S1530-891X(25)00031-X. https://doi.org/10.1016/j.eprac.2025.01.007.

