Urogenital Tuberculosis: 32 Cases
Abdellah Nachid, Anas Tmiri*, Mehdi Bennani, Adil Kbirou, Amine Moataz, Mohamed Dakir, Adil Debbagh, Rachid Aboutaieb
Urology Department, Ibn Rochd University Hospital, Casablanca, Morocco
Faculty of Medicine and Pharmacy Casablanca, Morocco
Received Date: 16/06/2025; Published Date: 18/07/2025
*Corresponding author: Anas Tmiri, Urology Department, Ibn Rochd University Hospital, Casablanca, Morocco; Faculty of Medicine and Pharmacy Casablanca, Morocco
Abstract
Tuberculosis is an infectious disease caused by strict aerobic acid-alcohol-resistant bacteria, mainly represented by mycobacterium tuberculosis.
Urogenital tuberculosis accounts for 4.5% to 27.2% of extra-pulmonary forms of tuberculosis, ranking 5th after pleural, lymph node, meningeal and osteoarticular forms. This pathology is always under-diagnosed. The progression of the disease, the evolution of lesions and tissue damage, is the result of a delay in diagnosis that can lead to CKD. Early diagnosis is the only guarantee of optimal management.
The aim of our work is to analyze the epidemiological, clinical, radiological and therapeutic features of patients with urogenital tuberculosis.
We present a case series of 32 patients treated for urogenital tuberculosis over a period of 6 years in the urology and infectious diseases departments at CHU IBN ROCHD, Casablanca.
Keywords: Tuberculosis; Urogenital tuberculosis; Extra pulmonary tuberculosis; Positive diagnosis; Surgical treatment
Introduction
Tuberculosis is an infectious disease caused by strict aerobic acid-alcohol-resistant bacteria, mainly represented by Mycobacterium tuberculosis. Bovine tuberculosis is caused by Mycobacterium bovis (around 5% of human tuberculosis cases). It affects various organs.
Only pulmonary tuberculosis is contagious via pflugal droplets [1].
Extrapulmonary tuberculosis (EPT) represents a very diverse group of pathologies. Urogenital localization ranks 5th after pleural, lymph node, bone and neuro-meningeal forms. Urogenital tuberculosis accounts for 4.5% to 27.2% of extra-pulmonary forms of tuberculosis [2,3].
We present a case series of 32 cases of urogenital tuberculosis.
The aim of our work is to analyze the epidemiological, clinical, radiological and therapeutic features of patients with urogenital tuberculosis.
Materials and Methods
Patients
1/ Date and place of study: The study was carried out at the Urology Department and Infectious Diseases Department of CHU IBN ROCHD in Casablanca over a 6-year period from March 1(st),2016 to June 30, 2022.
2/ Patient recruitment: The diagnosis of urogenital tuberculosis was based on the presence of at least one of the following:
- Bacilluria on ECBU with tuberculous localization at time of
- Presence of BK in urine on direct examination and/or
- Radiological images suggestive of urogenital
- Classical anatomopathological lesions of tuberculosis on bladder biopsies or surgical
Methods
This is a retrospective study of the files of patients with urogenital tuberculosis, with or without other localizations. Epidemiological, clinical, paraclinical, therapeutic and evolutionary data were recorded in a data sheet.
For the elaboration of this work we based ourselves on :
- The registers of the Urology Department and the Infectious Diseases
- Patient
- Phone
Statistical analyses were performed using SPSS 20.0 software.
Results
Epidemiology:
1/ Age distribution of patients: During the study period, we recorded 32 cases of urogenital tuberculosis. The mean age of our patients was 41 years, with extremes ranging from 22 to 60 years and a standard deviation of 7 years (Figure 1).
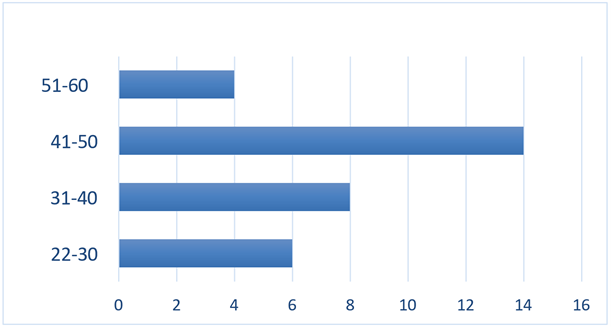
Figure 1: Distribution of patients by age.
2/ Distribution of patients by sex: There was a clear male predominance, with a sex ratio (M/F) of 1.66, i.e., 62.5% men and 37.5% women (Figure 2).
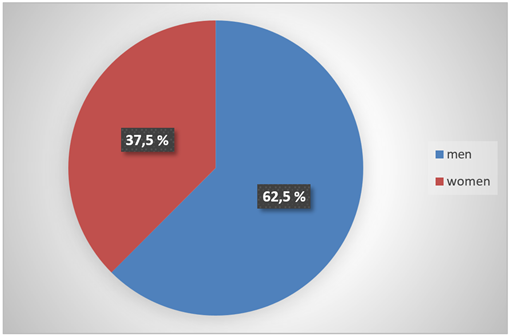
Figure 2: Distribution of patients by gender.
Clinical:
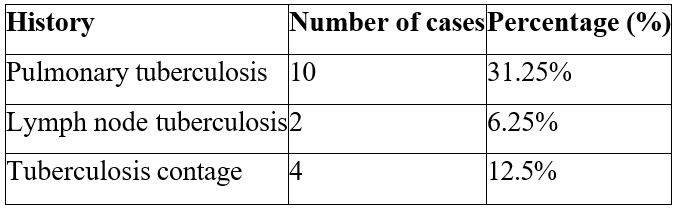
1/ Medical History: Extra-urinary tuberculosis was found in 12 patients (37.5% of all cases), pulmonary tuberculosis was associated with urogenital tuberculosis in 10 patients, and lymph node tuberculosis was found in 2 patients. The notion of family contact was identified in 4 patients (Table 1).
Table 1: Breakdown of patients' pathological histories.
2/ Duration of Symptomatological Evolution: The mean time to progression and consultation was 22 months, with extremes ranging from 4 to 37 months.
3/ Functional Signs: On admission, urinary burning and pollakiuria were the most frequent telltale signs, occurring in 22 patients (68.75%). 14 patients complained of low back pain, i.e. 43.75% of patients, and 12 patients had renal colic, i.e. 37.5% of patients. Genital signs, notably orchi- epididymitis and glans ulceration, were found in 10 patients (31.25% of cases).
4/ Physical Signs: General signs of tuberculosis (asthenia, anorexia, weight loss and night sweats) were found in 14 patients (43.75% of patients).
Lumbar tenderness was present in 16 patients (50%). An epididymal nodule was found in 6 patients (i.e. 18.75% of patients) and lumbar contact was positive in 6 patients (i.e.
18.75% of patients).
Paraclinical Examinations:
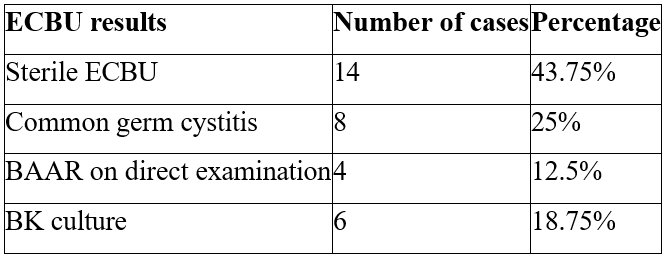
1/ ECBU: Urine was collected aseptically from morning urine, with fluid restriction for the preceding 12 hours. On 32 urine samples, direct examination and culture on specific media (LOWENSTEIN), carried out on 3 consecutive samples, gave the following results (Table 2):
Table 2: ECBU results.
2/ Tuberculin Intradermoreaction: The tuberculin intradermal test was not performed on any patients, as it was not available.
3/ Biology:
- / NFS: It was normal in 12 patients (37.5%), while inflammatory anemia and hyperleukocytosis were observed in 20 patients (62.5%).
- / Renal function: In our series, only two patients had renal failure, with elevated creatinemia figures of 22mg/l and 34 mg/l.
4/ Radiology:
- / UIV: It was carried out in 4 patients, showing pyelocalic dilatation and stenosis of the urethra on post-micturition imaging in two.
- / Uroscanner: 24 patients underwent a uroscanner, i.e. 75% of patients. The abnormalities found were as follows:
- Ureterohydronephrosis in 22 of our
- Calcium lithiasis with infiltration of peri-renal fat in 2
4.3 / Ultrasound: It was performed on all patients.
It revealed the following lesions (Table 3):
Table 3: Ultrasound abnormalities.

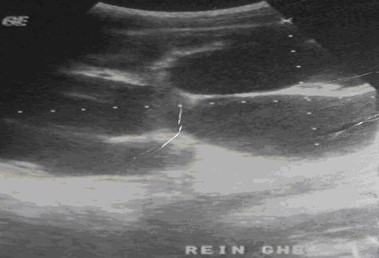
Figure 3: Major pyelo-caliceal dilatation with disappearance of the cortical index.
4.1 / Chest X-Ray: All our patients underwent chest radiography, which revealed 5 cases of pulmonary cavern and a pulmonary condensation image in three patients. It was normal in 24 cases.
5/ Cystoscopy with Biopsy: 6 patients underwent cystoscopy with biopsy, but the pathological examination was negative.
6/ Ureteroscopy with urine BK test: Carried out in 8 of our patients, showing staged strictures with the presence of BK on urine cytobacteriological examination.
7/ Anatomopathology:
Histological evidence of tuberculosis was obtained:
- Twice on lymph node
- Twice on a nephrectomy specimen, e. 6.25%.
Treatment
1/ Medical treatment: All our patients were put on specific antibacillary-based medical treatment for 6 months, combining four antibacillaries for 2 months: Isoniazid (5mg /Kg/ d), Rifampicin (10 mg/ Kg/ d), Pyrazinamide (30mg/ Kg/ d) and Ethambutol (20mg/ Kg/ d), followed by 2 antibacillaries: Isoniazid (5mg/ Kg/ d) and Rifampicin (10mg/ Kg/ d) for 4 months (2RHZE/4RH).
2/ Corticosteroid therapy: Corticosteroid therapy at a dose of 1 mg/kg/d was prescribed for 4 weeks in patients with stenosing lesions of the excretory tract or renal dilatation associated with double-J catheter rise.
3/ Surgical treatment: In our study, three patients underwent nephrostomy and four patients had JJ catheters inserted. Two patients (6.25%) underwent nephrectomy, with simple postoperative follow- up.
Evolution:
1/ Lost to view: 12 out of 32 patients were lost to follow-up.
2/ Relapses: There were no cases of tuberculosis relapse.
3/ Deaths: No deaths were recorded in our series.
Discussion
Tuberculosis is one of the leading infectious causes of death worldwide, and among HIV- positive patients. Its incidence is increasing, despite the national tuberculosis control program. Urogenital tuberculosis is characterized by its clinical polymorphism, which depends essentially on the location and course of the infection [4,5].
The mean age in our study was 41 years, with extremes ranging from 22 to 60 years. This mean is tending to increase in our country, following the national BCG vaccination program, which protects the young population, as well as the insidious evolution of the disease and the aging of the population. The average age was 38 in a study by Benchekroun et al. in Rabat [6] and 34 in the study by Bennani et al. in Casablanca [7].
Male predominance dominates in our study, with a sex ratio (M/F) of 1.6, i.e. 20 men vs. 12 women. This male predominance was present in several series: 62.5% of men in Benchekroun's series [6], 63% of men in Bennani's series [7], 56.1% of men in EL KHADER's series [8] and finally 73% of men in SOW's series [9].
Clinical polymorphism makes urogenital tuberculosis a late-reporting disease, which may be discovered at the stage of urological and nephrological sequelae, with a risk of renal failure or infertility [8,10].
In our study, the average delay between consultation and diagnosis was 22 months, which is in line with the literature, which reports a variable delay of between 12 and 24 months in 70% of cases, according to Bennani et al. [7]. Rabii et al [12] reported a delay of two years, depending on the site and progression of the disease, similar to the study by El Khader [8]. The delay can be even longer, ranging from 5 to 10 years [11].
In our series, cystitis was the most frequent revealing sign (68.75% of cases), which is in line with the literature, where cystitis remains the most frequent sign of discovery: 74.4% according to Bennani [7], 61.3% for El Khader [8]. Followed by isolated low back pain or renal colic. In our series, low back pain was present in 43.7% of cases, and renal colic in 37.5%.
These signs often point to an excretory tract obstruction or renal destruction [7,9,14]. It may be related to renal distension in cases of ureteral involvement.
Isolated genital involvement is uncommon, but urinary tract involvement is more common. Some 50-75% of men with genital involvement have radiological abnormalities of the urinary tract [13].
Its multiple localizations make tuberculosis a disease with a highly polymorphous clinical presentation [7,8]. The clinical examination may be normal, especially in women, and in the absence of accessible genital lesions in men. For El Khader [8], in his series of 57 cases, genital signs are present in 36.7% of cases. They are manifested by an epididymal nodule of the tail and/or epididymal head, or induration of the entire epididymis giving the appearance of a helmet crest, subacute orchiepididymitis with or without scrotal fistula, chronic prostatitis and hydrocele secondary to tuberculous pachyvaginitis.
In our series, examination of the genitalia revealed an abnormality in 31.2% of cases.
Diagnosis is often delayed [7,16]. Benabdellah asserts that only the conjugation of Three methods - bacteriology, histology and radiology - are used for diagnosis.
It is based on :
- The discovery of koch's bacillus in urine on direct examination or after culture on Lowenstein's If correctly and patiently investigated, it is found in 72% to 83% of cases [13,16]. PCR nuclear amplification techniques can be used to detect mycobacterial DNA. These are less sensitive than culture, but highly specific. Probes are available to identify clones [17].
- Urological images suggestive of tuberculosis [12] :
- Renal: pyelocecal dilatation, caliceal stenosis or amputation, renal pelvis retraction, cavern, small pyelonephric kidney or destroyed kidney (mastic kidney, mute kidney).
- Ureteral stenosis: often multiple, moniliform stenosis with significant
- Urethral: urethral
- The discovery on surgical specimens of the classic anatomopathological stigmata of the disease [18,19].
In our series, BAARs were found on direct examination in 4 patients, and culture was positive for BK in 6. El Khader [8] found a positive ECBU in 5.2% of patients in his series of 57 patients. Proof of the tuberculous nature of urogenital lesions was obtained in 8.8% of cases on bacteriological grounds (5 times): isolation of BK in urine (3 times) and in abscess pus (2 times) [8].
The seriousness of urogenital tuberculosis lies in the extent of the renal lesions and its bilaterality, or when it occurs on a single anatomical or functional kidney, which compromises renal function, or when the involvement is immediately manifested by acute or chronic renal failure. Fekak [15] described a rare and severe case of obstructive anuria of tuberculosis origin in a single anatomical kidney.
The diagnosis of anuria was based on the absence of diuresis. Ultrasound confirmed the obstructive nature of the anuria, and enabled puncture of the kidney and placement of a percutaneous nephrostomy, for diagnostic and therapeutic purposes, by performing a descending nephrography. BK testing was positive.
Two of our patients had renal failure. Hence the importance of early diagnosis before reaching the stage of renal failure.
The treatment of urogenital tuberculosis has the following objectives:
- The eradication of Koch's bacillus by medical treatment based essentially on
- Reconstructive surgery to treat after-
- Urogenital tuberculosis can never be treated without diagnostic proof. Hence the importance of bacteriological or anatomopathological proof. Every excisional specimen must therefore be subjected to a histological study and bacteriological culture, with antibiotic susceptibility testing as a matter of course.
- The discovery of the major anti-tuberculosis drugs, in particular Rifampicin, has totally altered conventional protocols and encouraged the use of shorter treatment regimens. Currently, two therapeutic regimens of 6 and 9 months are used, depending on whether 3 or 4 antibacillaries are used. These shorter treatment regimens have the advantages, among others, of being well tolerated, reducing the duration and cost of treatment, and improving patient compliance [20].
The basic rules for using these drugs are :
- The judicious combination of at least three antibacillary agents during the initial phase of treatment, with the aim of reducing the bacillary population in the lesions as early as possible.
- Sufficient treatment
- Taking medication
- A single dose of antibacillaries taken on an empty According to LE Guillou [20], two treatment regimens are currently in use:
- 1st diagram (6 months) :
The patient receives a daily dose of 4 anti-tuberculosis drugs for 2 months:
Isoniazid (5mg/kg), rifampicin (10mg/Kg), Ethambutol (20mg /kg) and Pyrazinamide (30mg/Kg). Thereafter, only Isoniaside and rifampicin are administered for 4 months at the same dosage.
- 2nd pattern (9 months):
For 2 months, the patient receives a daily dose of 3 antibacillaries: Ethambutol (20mg/Kg), isoniazid (5mg/kg) and rifampicin (10mg/kg). Ethambutol is then discontinued and the other 2 are administered for up to 9 months at the same dosage.
It appears that in either regimen, and despite their cost, rifampicin and isoniazid remain the mainstays of anti-tuberculosis chemotherapy.
In Benchekroun's study [13], 2 patients were treated with a 6-month regimen, divided into 2 phases: an initial phase combining streptomycin, isoniazid, rifampin and pyrazinamide 3 days out of 7 for 2 months, and a maintenance phase combining isoniazid and rifampin 6 days out of 7 for 4 months.
According to Bennani [7], short regimens are even more applicable to TUG than to pulmonary tuberculosis, because there are far fewer bacilli in renal lesions than in pulmonary lesions, and because of the richness of the renal vascularization, which enables antibacillaries to reach very high concentrations in the closed cavities of the kidney.
Some authors use rifampicin and isoniazid alone for 9 months, while others prefer to combine them with ethambutol. Nevertheless, the combination of SRHZ for 2 months followed by R and H for 7 months (2 SHRZ/7RH) seems to give the best therapeutic results [7].
According to Benabedlah [16], medical treatment enables rapid irradiation of the Koch's bacillus in most cases, but only cures the disease without sequelae in 20% of cases.
In Sow's series [9], the duration of treatment was 6 months for 17 patients, with four anti- tuberculosis drugs for 2 months: Streptomycin, Isoniazid, Rifampicin and Pyrazinamide, followed by 4 months of Rifampicin and Isoniazid. Six patients received intermittent treatment for 12 to 24 months [9]. The results of this therapeutic approach were not reported in the study.
For Fekak [15], with short regimens, relapses and resistance are virtually non-existent. The combination of streptomycin, rifampicin, isoniazid and pyrazinamide for 2 months, followed by R and H for 7 months (2 SHRZ/7RH) seems to give the best results.
Throughout the course of treatment, close collaboration between urologists and pulmonologists is essential to detect any scarring lesions that may be part of the "Couvelaire" disease [12].
Medical treatment for children must be adapted to their weight. The addition of streptomycin is indicated if Koch's bacillus is present in the urine. Treatment must be continued for 12 months
As far as adjuvant treatment is concerned, corticosteroid therapy has never proved effective in preventing excretory tract stenosis. At most, corticosteroids may be beneficial in cases of acute tuberculous cystitis. However, it is important to remember that rifampicin, as an enzyme inhibitor, affects the metabolism of corticosteroids and reduces their efficacy and bioavailability, hence the need to prescribe them in high doses [7].
Vitamin therapy is useful in combination with antibacillary treatment, especially vitamins B1 and B6, which reduce the side effects of antibacillary chemotherapy. The antioxidant effect of vitamin E in urogenital tuberculosis reduces the risk of urinary lithiasis formation, as reported by Srinivasan [21].
Despite the remarkable efficacy of medical treatment, surgery remains a vital part of the management of urogenital tuberculosis. It is necessary in 53% to 83% of cases, thus complementing medical treatment [16].
In Merrot's study [22], it was performed in 70% of cases for sequelae, with a 45% rate of nephrectomy.
Gupta [23], in a series of 241 cases over 17 years, performed 248 surgical procedures, with some patients requiring more than one procedure: 33 endoscopies, 87 exereses and 128 reconstructions.
In El Khader's series [8], surgical treatment was necessary in 75% of cases, and endo- urological maneuvers were required in 26.3% of cases.
Benchekroun [6], which included 48 cases of confirmed urinary tuberculosis, surgical treatment was recommended in 55% of cases, with a failure rate in 25%. Conservative treatment was recommended in 45% of cases, but failed in 48%. This high risk of both medical and surgical failure is due firstly to delayed diagnosis, then to nutritional status and unfavorable socio-economic conditions [25].
Rizzo [24] compared the incidence of surgery for urinary tuberculosis in his training between the periods: 80-89 and 90-99 - it was 0.67% in the former period, and 0.32% in the latter. There was a clear reduction in the use of surgery. This can be attributed to the effectiveness of antibacillary drugs, and to early diagnosis before the disease reaches the sequelae stage.
In our series, only 9 patients (i.e., 28% of all patients) required surgery or endo-urological intervention. This reflects the progress made in medical treatment and early diagnosis of this disease.
Conclusion
Tuberculosis is a curable and preventable disease, yet it is one of the leading infectious causes of death worldwide.
Between 15% and 40% of all people infected annually have extra-pulmonary tuberculosis. Urogenital tuberculosis ranks 5th after pleural, lymph node, meningeal and osteoarticular forms.
This pathology is always under-diagnosed. The progression of the disease, the evolution lesions and tissue damage, is the result of a delay in diagnosis that can lead to CKD.
Telltale signs often include chronic inflammation of the urinary tract, hematuria, isolated pyuria, impaired renal function, obstructive uropathy, infertility or renal or testicular mass.
Early diagnosis is the only guarantee of optimal care. Treatment should follow WHO recommendations.
References
- Watfa J, Michel Prog Urol, 2005; 15: 602-603.
- Peto HM, Pratt RH, Harrington TA, LoBue PA, Armstrong LR. Epidemiology of extrapulmonary tuberculosis in the United States, 1993-2006. Clin Infect Dis, 2009; 49: 1350-1357.
- Solovic I, Jonsson J, Korzeniewska-Koseła M, Chiotan DI, Pace-Asciak A, Slump E, et al. Challenges in diagnosing extrapulmonary tuberculosis in the European Union, 2011. Euro Surveill, 2013; 18: 1-9.
- WHO Global Tuberculosis report, 2018.
- The top 10 causes of death, 2019.
- Benchekroun A, Lachkar A, Soumana A, Farih MH, Belahnech Z, Marzouk M, et al. Urogenital tuberculosis a propos de 80 Annales d'urologie, 1998; 32(2): pp 60-88.
- Bennani S, Fekak H, Hafiani M, Debbagh A, El Moussaoui A, El Mrini M, Benjelloun Urogenital tuberculosis. A propos de 109 cas. Méd Mal infect, 1999; 29: 19-25.
- El Khader Khalid, Lrhorfi My Hfid, El Fassi Jamal, Tazi Karim, Hachim Mohamed, Lakrissa Urogenital tuberculosis. A 10-year experience. Progrès en Urologie, 2001; 11: 62-67.
- Sow Urogenital tuberculosis in Youndé. Aspects cliniques, para cliniques et thérapeutiques, à propos de 23 cas. Médecine d'Afrique noire, 1996; 43(10).
- El Mejjad Amine, Fekak Hamid, Debbagh Adil, Joual Abdenbi, Bennani Saad, El Mrini Renal adenocarcinoma on tuberculous nephritis. Progrès en Urologie, 2005; 15: 309-311.
- Mortier E, Pouchot J, Boussougant Y, Vinceneux Faut'il encore chercher le bacille de Koch dans les urines. Rev Médecine interne, 1997; 18: 193-194.
- Roudouane Rabii, Moufid Kamal, Joual Abdenbi, Maani Ahmed, Bennani Saad, El Mrini Pseudotumoral form of urinary tuberculosis. Progrès en urologie, 2007: 12: 1284-1287.
- Benchekroun A, Nouini Y, Annoud M, Moustapha A, Marzouk M, Faik M, et al. Epididymal tuberculosis: a case report with particular appearance on color echodoppler. Annales d'urologie, 2002; 36: 384-387.
- El Khader K, El Fassi J, Karmouni T, Tazi K, Ibnattya A, Hachimi M, et al. Urogenital tuberculosis, a propos of 40 Ann Urol, 1997; 31(6-7): 339-343.
- Fekak H, Rabii R, Moufid K, Joual A, Debbagh A, Bennani A, et al. Rare cause of obstructive anuria: Urogenital Annales d'urologie, 2003; 37: 71-74.
- Benabdellah A, Attar A, Maalem A, Bekkhoucha Meningeal tuberculosis and renal lithiasis. A propos d'un cas. Annales d'urologie, 2002; 36: 26-28.
- Eichbaum Q, Rubin E Tuberculosis. Advances in labatory dignosis and drug susceptibility testing . Am. J. Clin. Pathol, 2002; 118: S3-17.
- Bennani S, Aboutaieb R, El Mrini M, Benjelloun Place of corticotherapy and endoscopy in the treatment of urogenital tuberculosis. Ann Urol, 1994; 28: 243-249.
- Benchekroun A, Lachkar A, Soumana A, Farih M H, Belahnech Z, Marzouk M, et al. La tuberculose urogénitale a propos de 80 Annales d'urologie, 1998; 32(2): pp 60-88.
- Le Guillou M, Pariente J-L, Gueye S-M. Urogenital Encycl. Méd. Chir. Néphrologie- Urologie, 1998; 18-078-A-10.
- Sirinivasan S, Pragasam V, Jenita X, Kalaiselvi P, Muthu V, Varalakshmi Oxidative stress urogenital tuberculosis patients, a predicting factor for renal stone Formation amelioration by vitamin E suplementation. Clinica-chimica Acta, 2004; 350: 57-63.
- Merrot Thierry, Lachhaab Mustapha, Zerhouni Hicham, Alessandrini Urinary tuberculosis in children. A propos d'une forme sévère avec 19 ans de recul. Progrès en urologie, 2002; 12: 658-662.
- Gupta NP, Kumar R, Mundada OP, Aron M, Hemal AK, Dogra PN, Seth Reconstructive surgery for de management of genitourinary tuberculosis a single center experience. J.Urol, 2006; 175(6): 2150-2154.
- Rizzo M, Ponchietti R, Diloro F, Scelzi, Bongini A, Mondaini Twenty-years experience on genitourinary tuberculosis. Arch Ital urol Androl, 2004; 76(2): 83-87.
- Benchekroun TS, Kriouil A, Belkacem A, Jorio-Benkhraba M, El Fakir Y, Benhmmou M, et al. Urogenital tuberculosis in children Arch padiatr, 1997; 4: 857-

