Intraindividual Comparison of novel 18F-PSMA-1007 and 18F-AlF-PSMA-HBED-CC PET/CT in the Prospective Evaluation of Prostate Cancer Patients with Biochemical Relapse
Gerardo Gabriel dos Santos Loureiro1,2,*, Pablo Duarte Couto1, Juan Pablo Gambini Gonzalez1,2 and Omar Alonso Nuñez1,2
1Uruguayan Center of Molecular Imaging (CUDIM), Montevideo, Uruguay
2Nuclear Medicine and Molecular Imaging Center, Clinical Hospital, University of Uruguay, Montevideo, Uruguay
Received Date: 05/06/2025; Published Date: 10/07/2025
*Corresponding author: Gerardo Gabriel dos Santos Loureiro, MD, PhD, Uruguayan Center of Molecular Imaging (CUDIM), Montevideo, Uruguay; Nuclear Medicine and Molecular Imaging Center, Clinical Hospital, University of Uruguay, Montevideo, Uruguay
Abstract
Introduction: Among several 18F-labeled prostate-specific-membrane-antigen (PSMA) targeted PET/CT tracers, the recently introduced 18F-PSMA-1007 had demonstrated interesting properties for the diagnostic evaluation of prostate cancer (PCa), as outstanding tumor uptake and minimal excretion through the urinary-tract.
A novel radiotracer: [18F]AIF-PSMA-HBED-CC (18F-AlF-PSMA-11), was produced in our Centre, with suitable radiochemical purity for clinical purposes and with the advantage of low cost.
The aim of this study was to prospectively compare the image quality and the diagnostic values of both tracers in a sample of PCa patients at biochemical relapse.
Materials and Methods: A sample of 18 patients (median age: 69.5; median PSA level: 1.28 ng/mL; range: 0.01-25.4 ng/mL; Gleason Score >6) with biochemical recurrence after radical prostatectomy (n=9, 50%) or radiotherapy were prospectively included between July-August 2020. Within 1-2 weeks they underwent a PET/CT scan with 18F-PSMA-1007 and with 18F-AlF-PSMA-11, randomly performed, with a 16 or 64-slice PET/CT with TOF correction, 120 or 60 minutes after the administration of 4.2 and 4.07 MBq/Kg, respectively. Normal-organ biodistribution and tumor uptake between tracers were examined using the maximum SUV (SUVm). Correlative imaging, histopathology and/or clinical follow-up were considered as reference standard. Sensitivity and specificity were calculated.
Results: The normal organ biodistribution of 18F-PSMA-1007 and 18F-AlF-PSMA-11 has proven highly similar to other PSMA-targeted radiotracers, such as PSMA-617, DCFBC and DCFPyL. 18F-PSMA-1007 and 18F-AlF-PSMA-11 PET/CT demonstrated abnormal findings in 15 and 13 patients (positivity rate: 83% and 72%), respectively. At least one suspicious lesion for prostate cancer metastasis was detected in 13 (72%) and 11 (61%) of 18 patients, for each tracer respectively. A total of 157 lesions were detected by at least one radiopharmaceutical in the following sites: bone (n=120), lymph-nodes (n=20), prostate (n=9), lung (n=7) and brain (n=1); adding a total of 142 for 18F-PSMA-1007 and 143 for 18F-AlF-PSMA-11. Discriminating by radiotracer in the total population, PET/CT with 18F-PSMA-1007 and 18F-AlF-PSMA-11 identified 105 and 115 bone lesions, 20 and 15 lymph node lesions, 9 and 6 prostate lesions, 7 and 6 lung lesions and 1 brain lesion both, respectively.
Metastatic nodes as small as 1 mm in diameter were discovered.
For concordant lesions (n=127), we did not find a significantly different SUVm for both tracers: 14.8 (2.6-107.4) and 13.7 (2.5-75.3), median (range), for 18F-PSMA-1007 and 18F-AlF-PSMA-11, respectively (p=0.13). However, a significant correlation was found among both tracers’ SUVm (r = 0.94, n = 127, P< 0.00001). We found a significantly higher SUVm for 18F-AlF-PSMA-11 in concordant bone lesions (n=100, P<0.0001) and for 18F-PSMA-1007 in lymph-node concordant lesions (n=14, P=0.011), while no significant differences were found in prostate and soft tissue lesions. 18F-AlF-PSMA-11 had renal clearance and 18F-PSMA-1007 had hepatobiliary clearance. Uptake was significantly higher for 18F-AlF-PSMA-11 than for 18F-PSMA-1007 in the kidneys (median SUVm, 46.2 vs. 25.9; p=0.0012) and urinary bladder (median SUVm, 71.2 vs. 5.1; p=0.0003), whereas 18F-PSMA-1007 showed significantly higher uptake in the liver (median SUV, 17.9 vs. 7.2; p=0.0003) and gallbladder (median SUVm, 22.8 vs. 2.2; p=0.0003). The detection rates for disease for PSA levels <1,28 and >1,28 ng/mL (median PSA of our sample) was 66% and 100% por 18F-PSMA-1007, and 55% and 88%, for 18F-AlF-PSMA-11, respectively.
On a per patient basis the sensitivity and specificity values with their 95% C.I. were 0.93 (CI: 0.68 - 0.99) and 0.66 (95% CI: 0.09-0.99) for 18F-PSMA-1007; and 0.84 (CI: 0.54 - 0.98) and 0.60 (95% CI: 0.14-0.94) for 18F-AlF-PSMA-11, respectively.
Conclusion: 18F-PSMA-1007 and 18F-AlF-PSMA-11PET/CT seem to be clinically equivalent imaging techniques and have relevant sensitivity for the detection of PCa lesions. Low urinary excretion of 18F-PSMA-1007 present clear advantage for pelvic interpretation.
Keywords: Prostate cancer; Biochemical recurrence; 18PSMA-1007; 18AlF-PSMA-11; PET/CT; PSMA imaging
Introduction
Prostate cancer (PCa), ranks as the second most common cancer among men and is one of the most widespread malignant tumors globally, currently showing a high rate of occurrence and new cases [1].
Biochemical recurrence (BCR) refers to the rise in serum PSA levels following treatments that were aimed at curing the disease. This happens in around 30% of individuals who undergo radical prostatectomy (RP) and in 60% of those who receive external beam radiotherapy (EBRT) [2].
Traditional imaging methods like computed tomography (CT), bone scintigraphy (BS), and magnetic resonance (MR) displayed low precision rates when it came to restaging patients with BCR [3].
Positron emission tomography/computed tomography (PET/CT) with 11C and 18F-Choline has found widely use for the evaluation of PCa patients but showed globally a suboptimal sensitivity at early BCR. Thus, new tracers with better performance were needed [4].
The introduction of ligands targeting prostate-specific membrane antigen (PSMA) has changed the management of patients with prostate cancer (PCa) [4].
In addition to the well-known overexpression of PSMA, its internalization after binding is actually being used for a theragnostic approach (177Lutetium) [5].
68Ga-PSMA-HBED-CC (68Ga-PSMA-611, ABX) PET/CT has been proposed as a promising tracer for imaging patients with biochemical recurrence with the potential of changing clinical management, specially at low PSA levels, performing better than the previously approved tracer: radiolabelled choline [4].
However, 68Ga-labelled compounds have limitations including short half-life, non-ideal energies, expensive generators’production with limited activity per synthesis (one to four patients per batch), and rapid excretion via the urinary tract [6].
18F-labelled PSMA ligands are of major interest and have several principal advantages over 68Ga-PSMA-11, including production in large scales by a cyclotron, lower positron energy, higher image quality, and possibility of delayed images [7].
Among several 18F-PSMA-ligands like 18F-DCFBC or 18F-DCFPyL, the most recently 18F-PSMA-1007 had demonstrated interestingly properties as high labelling yields, outstanding tumor uptake and fast and non-urinary background clearance [6,8].
Although several studies recommend the use of PSMA PET/CT for localization of prostate cancer in the setting of BCR, the indication for initial staging at primary diagnosis is actually well documented, buy also actually its indication in initial staging is well established [10]. This was also reported by our group [11].
The aim of this study was to compare the diagnostic values of 18F-PSMA-1007 vs 18F-AlF-PSMA-11 in patients with prostate cancer and biochemical relapse after initial treatment.
Material and Methods
Patient characteristics: A sample of 18 patients (median age: 69.5, range: 54-80 years; median PSA level: 1.28 ng/mL; range: 0.01-25.4 ng/mL; Gleason Score >6) with biochemical recurrence after radical prostatectomy (n=9, 50%) or radiotherapy were prospectively included between July-August 2020.
Compliance with Ethical Standards: This study was approved by the Ethics Committee of our Centre and conducted according to the 1964 Helsinki Declaration and its later amendments or comparable ethical standards. Additionally, informed consents and consents to publish were obtained from all individual participants included in the study.
Radiopharmaceuticals:
18F-PSMA-1007: "The 18F isotope was produced via the nuclear reaction 18O(p,n)18F in a PETTrace cyclotron (GE). The synthesis of [18F]F-PSMA-1007 was conducted on a FASTLab automated synthesis platform (GE), housed within an MIP1 hot cell (Comecer).
Quality control was performed in accordance with the monograph established in EP 11.0 (07/2021:3116). All reagents used for synthesis and quality control were procured from ABX (Germany)."
18F-AlF-PSMA-11: The complex [18F]AlF-PSMA was obtained from an automated Tracerlab FXFN® (GE) platform.
The radiopharmaceutical was achieved with a radiochemical purity higher than 90% and with a radiochemical purity of 95 ± 3%. The product verified stability in the final formulation vial during 4 h and in human plasma up to 1h [9].
Imaging:
Within 1-2 weeks all patients underwent a PET/CT scan with 18F-PSMA-1007 and with 18F-AlF-PSMA-11, randomly performed, with a 16 or 64-slice PET/CT with TOF correction 120 or 60 minutes after the iv administration of 4.2 and 4.07 MBq/Kg, respectively.The images were acquired from skull to mid-thigh.
The acquisition and processing parameters of PET images were the same for both tracers. CT parameters: tube voltage 120 kVp, autoMA 80-180 mA, index noise 30, “GE SmartMa dose modulation”, rotation time 0.8 sec, rotation length - full helical thickness: 3.75 mm, Pitch 1.375:1 and speed 55 (mm/rot). PET data were acquired in 3D with a scan duration of 3 minutes per bed position and with 11-slice overlap. Images were reconstructed using an ordered subset expectation maximization algorithm (OSEM) with time-of-flight correction (matrix size 128 x 128 pixels) with 2 iterations/24 subsets.
Image Analysis
Images were evaluated by two board-certified specialists in nuclear medicine and by one board-certified radiologist, resolving any disagreements by consensus. 18F-PSMA-1007 and 18F-AlF-PSMA-11 PET/CT scans were randomly evaluated.
Circular regions of interest were placed on representative slices of the liver, spleen, kidney, urinary bladder, gallbladder, parotid glands, salivary glands and lacrimal glands, as well as in malignant lesions. This way, normal-organ biodistribution and tumor uptake in all abnormal foci between tracers were examined using the maximum standardized uptake value (SUVm).
Suspicious metastatic lesions were defined as any abnormal focal uptake at one or more locations, not related to normal tracer biodistribution, higher than the surrounding background or compared with normal tissue, localized by hybrid images, excluding joint processes and areas of physiological uptake.
Metastasis were registered and evaluated regarding their localization (prostate, bone, lymph node-LN- or soft tissue metastases) and their SUVm.
Gold Standard @ follow up
Histopathology (when available), correlative imaging and/or clinical follow-up were considered as reference standard. Our validation criteria data was:
- Histopathologic analysis.
- Multiple lesions of metastatic appearance.
- Increase of the PSA and/or pathological PET or conventional studies in untreated patients in follow-up.
- Decrease of the PSA and/or improvement of lesions in PET or conventional studies after the specific treatment of the disease.
- Unequivocal positive findings at baseline that persist during follow-up in a setting of PSA >0.2 ng/mL, at least three weeks following prostatectomy.
Statistical analysis
We carried out a comparison between results obtained with both tracers regarding the number of detected PET lesions, SUVm in normal tissues and malignant lesions (in prostate bed, lymph nodes and extranodal lesiones), and the PSA.
We used the non-parametric Spearman's Rho test and the Pearson´s correlation coefficient to measure the strength of association between SUVmax in all concordant lesions.
SUVm values from the same lesions in both 18F-PSMA-1007 and 18F-AlF-PSMA-11 studies were statistically analysed using a nonparametric two-sided Wilcoxon signed rank tests and the student paired t-test.
Sensitivity and specificity were selected to describe the diagnostic performance of PET/CT in detecting tumor involvement.
A P value <0.05 was considered significant.
For statistical analyses, we used the Statistical Package for the Social Sciences (SPSS) version 23.
Results
There were no symptoms or side effects in any patient post-injection of the radiotracer.
The normal organ biodistribution of 18F-PSMA-1007 and 18F-AlF-PSMA-11 has proven highly similar to other PSMA-targeted radiotracers, such as PSMA-617, DCFBC and DCFPyL.
Images of both tracers were of high visual quality.
18F-PSMA-1007 and 18F-AlF-PSMA-11 PET/CT demonstrated abnormal findings in 15 and 13 patients (positivity rate: 83% and 72%), respectively. At least one suspicious lesion for prostate cancer metastasis was detected in 13 (72%) and 11 (61%) of 18 patients, for each tracer respectively.
The detection rates for disease for PSA levels <1,28 and >1,28 ng/mL (median PSA of our sample) was 66% and 100% por 18F-PSMA-1007, and 55% and 88%, for 18F-AlF-PSMA-11, respectively.
A total of 157 lesions were detected by at least one radiopharmaceutical in the following sites: bone (n=120), lymph-nodes (n=20), prostate (n=9), lung (n=7) and brain (n=1); adding a total of 142 for 18F-PSMA-1007 and 143 for 18F-AlF-PSMA-11. Discriminating by radiotracer in the total population, PET/CT with 18F-PSMA-1007 and 18F-AlF-PSMA-11 identified 105 and 115 bone lesions, 20 and 15 lymph node lesions, 9 and 6 prostate lesions, 7 and 6 lung lesions and 1 brain lesion both, respectively.
Of notice 18F-PSMA-1007 PET/CT detected lymph node metastases in the pelvis, including nodes as small as 1 mm in diameter.
For concordant lesions (n=127), we did not find a significantly different SUVm for both tracers: 14.8 (2.6-107.4) and 13.7 (2.5-75.3), median (range), for 18F-PSMA-1007 and 18F-AlF-PSMA-11, respectively (p=0.13).
However, a significant correlation was found among both tracers’ SUVm (r = 0.94, n = 127, P< 0.00001).
We found a significantly higher SUVm for 18F-AlF-PSMA-11 in concordant bone lesions (n=100, P<0.0001) and for 18F-PSMA-1007 in lymph-node concordant lesions (n=14, P=0.011), while no significant differences were found in prostate and soft tissue lesions.
18F-AlF-PSMA-11 had renal clearance and 18F-PSMA-1007 had hepatobiliary clearance.
With regard to normal organs the biodistribution of the two tracers differed.
Uptake was significantly higher for 18F-AlF-PSMA-11 than for 18F-PSMA-1007 in the kidneys (median SUVm, 46.2 vs. 25.9; p=0.0012) and urinary bladder (median SUVm, 71.2 vs. 5.1; p=0.0003), whereas 18F-PSMA-1007 showed significantly higher uptake in the liver (median SUVm, 17.9 vs. 7.2; p=0.0003) and gallbladder (median SUVm, 22.8 vs. 2.2; p=0.0003). There were no significant differences comparing uptake in the spleen (median SUVm, 18.2 vs. 16.7; p<0.05). 18F-PSMA-1007 had statistically significant higher uptake in the salivary glands, parotid glands and lacrimal glands (median SUVm, 27.3 vs.17 .0, p=000.4; 17.9 vs 7.2, p=.0.0003 and 13.47 vs 9.9. p=0.0003 respectively).
On a per patient basis the sensitivity and specificity values with their 95% C.I. were 0.93 (CI: 0.68 - 0.99) and 0.66 (95% CI: 0.09-0.99) for 18F-PSMA-1007; and 0.84 (CI: 0.54 - 0.98) and 0.60 (95% CI: 0.14-0.94) for 18F-AlF-PSMA-11, respectively.
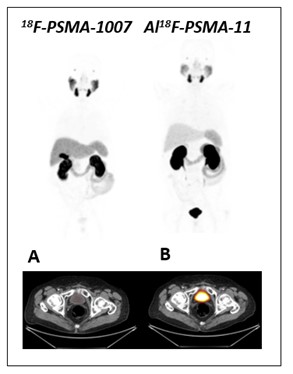
Figure 1: Normal biodistribution of 18F-PSMA-1007 and 18F-AlF-PSMA-11. MIP and axial PET/CT images of a prostate cancer patient showing no urinary excretion of 18F-PSMA-1007 (A) that enables excellent assessment of the prostate. Note that increasing accumulation in gallbladder and in the liver could limit the detection of unusual liver metastases). Besides, normal accumulation of 18F-AlF-PSMA in the urinary bladder (B) difficult interpretation.
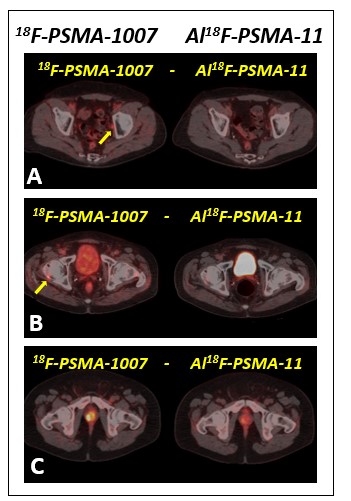
Figure 2: Axial PET CT images of three different prostate cancer patients showing metastasis in pelvic lymph node (A) and right femoral head (B) (yellow arrows) demonstrated only by means of 18F-PSMA-1007, and coincident prostate relapse (C). Note the better contrast and uptake intensity of 18F-PSMA-1007.
Discussion
In PCa individuals who underwent pretendly curative treatment and who experience biochemical recurrence, identifying where recurrent prostate cancer is located is crucial for planning subsequent treatments [12].
Following the identification of biochemical recurrence (PSA 0. 2 ng/ml), it is crucial to ascertain if it is localized or spread, as this influences the treatment options available, particularly for a specific group of patients who might qualify for curative salvage treatments. Traditional imaging methods like cross-sectional scans or bone scans have a low success rate in identifying these cases, particularly when serum PSA levels are low [13].
As a result, different radioactive markers are being researched to enhance the imaging of both recurring and initial cases of prostate cancer. So far, PSMA radioligands have emerged as the most accurate and precise for detecting prostate cancer, especially in patients at high risk for the disease [12].
PET/CT with 68Ga-PSMA has been proposed as a promising tracer for imaging patients with biochemical recurrence at low PSA levels with the potential of changing clinical management, performing better than the old gold-standard radiolabelled choline [4].
Also, the indication for detection of metastases for initial staging and its use in theragnosis-concept (177Lutetium) is rapidly being consolidating [5,10].
However, 68Ga labelled PSMA has several shortcomings such as limited availability for clinical use of the 68Ga generator, non-ideal energies, short half-life and a high urinary excretion, which can obscure detection of the primary or residual disease.
The introduction of 18F-labelled tracers has demonstrated promising results for the diagnostic workup of prostate cancer and seem to be an attractive alternative to 68Ga-PSMA-11 due to several principal advantages: availability of larger amounts of activity, a lower positron energy, higher image quality and possibility of delayed images.
An interesting tracer developed in our Centre: 18F-ALF-PSMA-11, can be produced on a large scale with suitable radiochemical purity for clinical purposes.
This tracer has been suggested as a novel and attractive alternative to 68Ga-PSMA-11 and others 18F-PSMA tracers with accessibility and commercial advantages as well as similar tumour uptake among them and the additional advantage of low cost. Notable a recent paper made a head-to-head comparison between 18F-AlF-PSMA-11and 68Ga-PSMA-11, performing in a comparable way [9].
18F-PSMA-1007 is a novel PSMA ligand that has excellent preclinical characteristics and that is only minimally excreted by the urinary tract, a potential advantage for pelvic imaging.
18F-PSMA-1007 had demonstrated properties as high labelling yields, outstanding tumor uptake and fast, non-urinary background clearance. This is interesting because most published studies investigated the diagnostic potential agents that are excreted renally.
We report the first experience at our center with 18F-PSMA-1007 identifying its advantages and potential applications and making a prospective comparation with 18F-ALF-PSMA-11 concerning image quality and diagnostic values of both tracers in a sample of PCa patients at biochemical relapse.
Our team was the first to improve the creation of an Al18F radiofluorinated GLU-UREA-LYS(AHX)-HBED-CC PSMA ligand using an automated synthesis system. This process achieved a good level of radiochemical purity that is acceptable for clinical use, and it also offered the benefit of being affordable [9].
A head-to-head comparison between 18F-AlF-PSMA-11 and 68Ga-PSMA-11 demonstrated good performance of both tracers in diagnosing PCa [14].
In this prospective study were included 18 patients with biochemical recurrent PCa (median age: 69.5, range: 54-80 years; median PSA level: 1.28 ng/mL; range: 0.01-25.4 ng/mL; Gleason Score >6) who were previously treated with radical prostatectomy and/ or radiation therapy of prostate bed (50% each).
There were no side effects in any patient post-injection of the radiotracer.
The normal organ biodistribution of 18F-PSMA-1007 and 18F-AlF-PSMA-11 has proven highly similar to other PSMA-targeted radiotracers, such as PSMA-617, DCFBC and DCFPyL [6-8].
Images of both tracers were of high visual quality and most lesions showed high contrast, as show in the literature. In healthy subjects, it has been proven that the blood pool contained mean 12% of the 18F-PSMA-1007 injected dose at 2 h p.i. Also, clearance via the urinary tract was minimal and in average only 0.7 % of the injected activity were eliminated in the urine during the 2–4 h interval [8].
Overall detection rate was 83% (15/18) and 72% (13/18) for 18F-PSMA-1007 and 18F-AlF-PSMA-11 PET/CT, while distant metastasis was detected in 13 (72%) and 11 (61%) patients respectively.
These data are similar to previous reports concerning this PSMA ligand. In two studies sites of BCR were localized in 90 % of patients including those with modest elevations in prostate specific antigen (PSA) [15,16].
The detection rates for disease for PSA levels <1,28 and >1,28 ng/mL (median PSA of our sample) was 66% and 100% por 18F-PSMA-1007, and 55% and 88%, for 18F-AlF-PSMA-11, respectively.
Our findings align with earlier studies regarding these PSMA ligands.
Perera reviewed sixteen studies that included 1309 patients. The positive scan rates for PSA categories 0–0. 2, 0. 2–1, 1–2, and 2 ng/ml were 42%, 58%, 76%, and 95%, respectively. When analyzing by patient, both the overall sensitivity and specificity were found to be 86%. In terms of per-lesion analysis, the overall sensitivity and specificity were 80% and 97%, respectively [17].
Afshar-Oromieh and their team identified at least one prostate cancer-related lesion in 83% of the patients. They showed detection rates of 50% for patients with serum PSA levels at 0. 5 ng/ml and 58% for those with PSA levels between 0. 5 and 1 ng/ml [18].
An aggregated detection rate of 89. 5% was found in a consistent group of 248 patients after they underwent radical prostatectomy. The detection rates for early biochemically recurrent cancer at PSA levels of 0. 2–0. 5 and 0. 5–1 ng/mL were recorded as 57. 9% and 72. 7%, respectively [16].
In an initial study on 68Ga-PSMA-IT, detection rates were noted to be 52% for PSA levels below 0. 5 ng/mL, 55% for levels between 0. 5 and 1. 0 ng/mL, 70% for levels between 1. 0 and 2. 0 ng/mL, and 93% for levels between 2. 0 and 5. 0 ng/mL [19].
Even though there were only a few patients involved, this research supports a strong detection rate for both markers at low PSA levels in a planned trial setup.
A total of 157 lesions were detected by at least one radiopharmaceutical in the following sites: bone (n=120), lymph-nodes (n=20), prostate (n=9), lung (n=7) and brain (n=1); adding a total of 142 for 18F-PSMA-1007 and 143 for 18F-AlF-PSMA-11. Discriminating by radiotracer in the total population, PET/CT with 18F-PSMA-1007 and 18F-AlF-PSMA-11 identified 105 and 115 bone lesions, 20 and 15 lymph node lesions, 9 and 6 prostate lesions, 7 and 6 lung lesions and 1 brain lesion both, respectively.
In our research, 18F-PSMA-1007 PET/CT detected lymph node metastases in the pelvis, including nodes as small as 1 mm in diameter.
Giessel and his team were the first to describe that 18F-PSMA-1007 PET/CT could detect micrometastases in patients with Biochemically Recurrent Prostate Cancer at very low PSA levels providing critical information to correctly restaging disease and to discuss appropriate treatment options [20].
In our sample PET/CT with 18F-PSMA-1007 and 18F-AlF-PSMA-11 identified 20 and 15 lymph node lesions, respectively.
The same author demonstrated an excellent sensitivity of 94.7% with 18F-PSMA-1007 PET/CT in detecting lymph-node metastases in the pelvis, [21] performing better than 68Ga-PSMA-PET.(20, 22) This can be explained: as lymph node metastases with median diameters of 5-6 mm are close to the technical resolution limits of PET with 68Ga-PSMA tracers, it would be reasonable that 18F-PSMA tracers might perform at a higher level.
For concordant lesions (n=127), we did not find a significantly different SUVm for both tracers: 14.8 (2.6-107.4) and 13.7 (2.5-75.3), median (range), for 18F-PSMA-1007 and 18F-AlF-PSMA-11, respectively (p=0.13).
However, a significant correlation was found among both tracers’ SUVm (r = 0.94, n = 127, P< 0.00001).
We found a significantly higher SUVm for 18F-AlF-PSMA-11 in concordant bone lesions (n=100, P<0.0001) and for 18F-PSMA-1007 in lymph-node concordant lesions (n=14, P=0.011), while no significant differences were found in prostate and soft tissue lesions.
The increased absorption of 18F-AlF-PSMA-11 in bones can be understood. Lütje proposed that there is a slight instability that leads to Al18F absorption in bones, which could complicate interpretations and make it hard to see small prostate cancer bone metastases. Furthermore, the significant non-specific absorption in bones injected with 18F-AlF-PSMA-11 indicated a quick breakdown in living organisms, a finding that was supported by a plasma stability test conducted in a lab. To avoid the major time-related breakdown of 18F-AlF-PSMA-11, PET imaging should occur no later than one hour after injection. In our research, this was not an issue, and we were able to detect metastases using established standard criteria [23,24].
With regard to normal organs the biodistribution of the two tracers differed.
This is consistent with Giesel´s results who demonstrated distinct organ uptake for lacrimal glands, salivary glands, liver, spleen, small intestine and kidneys in healthy volunteers [8].
18F-AlF-PSMA-11 had renal clearance and 18F-PSMA-1007 had hepatobiliary clearance.
Statistically, uptake was significantly higher for 18F-AlF-PSMA-11 than for 18F-PSMA-1007 in the kidneys (median SUVm, 46.2 vs. 25.9; p=0.0012) and urinary bladder (median SUVm, 71.2 vs. 5.1; p=0.0003), whereas 18F-PSMA-1007 showed significantly higher uptake in the liver (median SUVm, 17.9 vs. 7.2; p=0.0003) and gallbladder (median SUVm, 22.8 vs. 2.2; p=0.0003). There were no significant differences comparing uptake in the spleen (median SUVm, 18.2 vs. 16.7; p<0.05). 18F-PSMA-1007 had statistically significant higher uptake in the salivary glands, parotid glands and lacrimal glands (median SUVm, 27.3 vs.17 .0, p=000.4; 17.9 vs 7.2, p=.0.0003 and 13.47 vs 9.9. p=0.0003 respectively).
The SUVmax values of normal organ biodistribution and tumor uptake examined, were similar to those reported in the literature. For example, the delineation of tumors improved at 3 h p.i reached an average SUVmax of 41 in the primary tumors [8].
It has been proben uptake was significantly higher for 18F-DCFPyL than for 18FPSMA- 1007 in the kidneys, urinary bladder, and lacrimal gland, hereas 18F-PSMA-1007 showed significantly higher uptake in the liver, gallbladder, spleen and salivary glands [25].
The 18F-PSMA-1007 PET/CT scan is effective in identifying recurrent prostate cancer in many patients experiencing biochemical relapse. Even in patients with a low PSA level of 0. 5 ng/ml or less, the chances of finding abnormal results on the 18F-PSMA-1007 PET/CT scan appears to be quite high, which could greatly influence how we treat this important group of patients.
The 18F-AlF-PSMA PET/CT method shows promise for assessing individuals with prostate cancer. In the later stages, a lower liver background might make acute liver failure more likely, particularly in the rare instances where liver metastases arise [26].
When we look at other PSMA-targeting PET tracers, the low amount of urine background in 18F-PSMA-1007 offers greater diagnostic benefits in PET/CT scans for assessing the prostate bed and pelvis in patients with recurrent prostate cancer. 18F-PSMA-1007 is at least as effective as 68Ga-PSMA-11, but its longer half-life, along with better energy properties and the absence of urinary excretion, helps to address certain practical challenges faced by 68Ga-labelled PSMA-targeted tracers [26].
Recently, researchers discovered that PSMA is present in the new blood vessels of various non-prostate solid tumors, such as cancers of the breast, bladder, colon, and kidney. This presence can affect the outcomes and change the precision of the method. In our research, one of the criteria for excluding patients was having additional tumors besides prostate cancer [27].
18F-PSMA-1007 and ALF operate in a way that is comparable to other PSMA-PET agents and also to other PET tracers that are labelled with 18F.
On a per patient basis the sensitivity and specificity values with their 95% C.I. were 0.93 (CI: 0.68 - 0.99) and 0.66 (95% CI: 0.09-0.99) for 18F-PSMA-1007; and 0.84 (CI: 0.54 - 0.98) and 0.60 (95% CI: 0.14-0.94) for 18F-AlF-PSMA-11, respectively.
Recent research has indicated that there can be times when radiolabeled PSMA uptake is higher in rib fractures and also in non-cancerous bone conditions like fibrous dysplasia and Paget's disease. These observations are important to note when presenting PET/CT findings, which is why the existence of non-cancerous diseases was a criterion for excluding cases in our clinical study [27].
While previous studies have mentioned false positives related to uptake in retroperitoneal celiac ganglia, we were able to identify these instances easily in this analysis, so they were not factored into our results [28].
Regarding inaccurate negative results from PET/CT, some researchers have suggested that the effectiveness of PET/CT might be affected by tiny lesions that are 5 mm, which they consider to be the main limitation of the method. In our findings, the tiniest lymph node identified was 7 mm [22].
There are some notable limitations in our study that should be acknowledged.
Due to ethical and practical constraints, we could not confirm individual lesions through histopathology. Instead, we classified the lesions using imaging techniques and/or clinical follow-up, as many other studies in the literature have also done [22,29].
There are discussions about how androgen deprivation therapy (ADT) influences how often PET/CT scans with 68Ga-PSMA-11 are detected, but evidence indicates that there is a notable connection between ongoing ADT and the chances of obtaining a pathological radiolabeled PSMA PET/CT scan. In cases of hormone-sensitive prostate cancer (HSPC), receiving ADT before treatment can result in reduced PSMA expression, which in turn diminishes the sensitivity of the radiotracer.
In the group of patients we studied, whether they had concurrent or prior ADT did not exclude them based on PSMA expression and tracer uptake, and its impact on the detection rate remains uncertain.
These tracers demonstrated good diagnostic performance similar to other 18F-labelled PET-tracers and overcame practical limitations of 68Ga-labelled PSMA targeted tracers. Also, their superior ability to detect recurrence missed by conventional imaging will have a significant impact on patient management.
Conclusion
18F-PSMA-1007 and 18F-AlF-PSMA-11PET/CT seem to be clinically equivalent imaging techniques and have relevant sensitivity for the detection of PCa lesions in the biochemical recurrence scenario that would impact patient management.
Low urinary excretion of 18F-PSMA-1007 present clear advantage for pelvic interpretation.
Further studies are needed to confirm these preliminary results.
References
- Ferlay J, Soerjomataram I, Dikshit R, et al. Cancer incidence and mortality worldwide: Sources, methods and major patterns in GLOBOCAN 2012. Int J Cancer, 2015; 136(5): E359–386.
- Khuntia D, Reddy CA, Mahadevan A, Klein EA, Kupelian PA. Recurrence-free survival rates after external-beam radiotherapy for patients with clinical T1-T3 prostate carcinoma in the prostate-specific antigen era: what should we expect? Cancer, 2004; 100(6): 1283-1292.
- Hövels AM, Heesakkers RAM, Adang EM, Jager GJ, Strum S, Hoogeveen YL, et al. The diagnostic accuracy of CT and MRI in the staging of pelvic lymph nodes in patients with prostate cancer: a meta-analysis. Clin Radiol, 2008; 63(4): 387–395.
- Afshar-Oromieh A, Zechmann CM, Malcher A, Eder M, Eisenhut M, Linhart HG, et al. Comparison of PET imaging with a (68)Ga-labelled PSMA ligand and (18)F-choline-based PET/CT for the diagnosis of recurrent prostate cancer. Eur J Nucl Med Mol Imaging, 2014; 41(1): 11-20.
- Kratochwil C, Giesel FL, Stefanova M, Benešová M, Bronzel M, Afshar-Oromieh A, et al. PSMA-Targeted Radionuclide Therapy of Metastatic Castration-Resistant Prostate Cancer with 177Lu-Labeled PSMA-617. J Nucl Med, 2016; 57(8): 1170-1176.
- Dietlein M, Kobe C, Kuhnert G, Stockter S, Fischer T, Schomäcker K, et al. Comparison of (18F)DCFPyL and (68Ga)Ga-PSMA-HBED-CC for PSMA-PET Imaging in Patients with Relapsed Prostate Cancer. Mol Imaging Biol, 2015; 17(4): 575–584.
- Mease RC, Dusich CL, Foss CA, Ravert HT, Dannals RF, Seidel J, et al. N-(N-((S)-1,3-dicarboxypropyl) carbamoyl)-4-(18F) fluorobenzyl-L- cysteine, (18F)DCFBC: A new Imaging probe for prostate cancer. Clin Cancer Res, 2008; 14(10): 3036–3043.
- Giesel FL, Hadaschik B, Cardinale J, Radtke J, Vinsensia M, Lehnert W, et al. F-18 labelled PSMA-1007: biodistribution, radiation dosimetry and histopathological validation of tumor lesions in prostate cancer patients. Eur J Nucl Med Mol Imaging, 2017; 44(4): 678-688.
- Giglio J, Zeni M, Savio E, Engler H. Synthesis of an Al18F radiofluorinated GLU-UREA-LYS(AHX)-HBED-CC PSMA ligand in an automated synthesis platform. EJNMMI Radiopharm Chem, 2018; 3(1): 4.
- Georgakopoulos A, Bamias A, Chatziioannou S. Current role of PSMA-PET imaging in the clinical management of prostate cancer. Ther Adv Med Oncol, 2023; 15: 17588359231208960.
- Dos Santos Loureiro GG, Duarte Couto P, Gambini Gonzalez JP, Alonso Nuñez O. Comparative Evaluation of (18F)AlF-PSMA-HBED-CC and 68Ga-PSMA-HBED-CC in Staging Intermediate-/High-Risk Prostate Cancer: A Prospective Study. World J Nucl Med, 2025; 24(2): 118-127. doi: 10.1055/s-0045-1801842.
- Giesel FL, Knorr K, Spohn F, Will L, Maurer T, Flechsig P, et al. Detection Efficacy of 18F-PSMA-1007 PET/CT in 251 Patients with Biochemical Recurrence of Prostate Cancer After Radical Prostatectomy. J Nucl Med, 2019; 60(3): 362-368. doi: 10.2967/jnumed.118.212233.
- Eiber M, Fendler WP, Rowe SP, et al. Prostate-specific membrane antigen ligands for imaging and therapy. J Nucl Med, 2017; 58(suppl 2): 67S–76S.
- EJNMMI Rep, 2024; 8(1): 28. doi: 10.1186/s41824-024-00217-5
- Afshar-Oromieh A, Avtzi E, Giesel FL, Holland-Letz T, Linhart HG, Eder M, et al. The diagnostic value of PET/CT imaging with the (68)Ga-labelled PSMA ligand HBED-CC in the diagnosis of recurrent prostate cancer. Eur J Nucl Med Mol Imaging, 2015; 42(2): 197-209. doi:1007/s00259-014-2949-6.
- EiberM, Maurer T, SouvatzoglouM, Beer AJ, Ruffani A, Haller B, et al. Evaluation of hybrid 68Ga-PSMA ligand PET/CT in 248 patients with biochemical recurrence after radical prostatectomy. J Nucl Med, 2015; 56(5): 668–674. doi:2967/jnumed.115.154153.
- Hoffmann MA, Miederer M, Wieler HJ, Ruf C, Jakobs FM, Schreckenberger M. Diagnostic performance of 68Gallium-PSMA-11 PET/CT to detect significant prostate cancer and comparison with 18FEC PET/CT. Oncotarget, 2017; 8(67): 111073–111083.
- Afshar-Oromieh A, Malcher A, Eder M, Eisenhut M, Linhart HG, Hadaschik BA, et al. Pet imaging with a [68ga]gallium-labelled psma ligand for the diagnosis of prostate cancer: Biodistribution in humans and first evaluation of tumour lesions. Eur J Nucl Med Mol Imaging, 2013; 40(4): 486–495.
- BerlinerC. Detection rate of PET/CT in patients with biochemical relapse of prostate cancer using [68Ga]PSMA I&T and comparison with published data of [68Ga]PSMA HBED-CC. Eur J Nucl Med Mol Imaging, 2017; 44: 670–677.
- Giesel FL, Kesch C, Yun M, Cardinale J, Haberkorn U, Kopka K, et al. 18F-PSMA-1007 PET/CT Detects Micrometastases in a Patient With Biochemically Recurrent Prostate Cancer. Clin Genitourin Cancer, 2017; 15(3): e497-e499. doi: 10.1016/j.clgc.2016.12.029.
- Giesel FL, Hadaschik B, Cardinale J, Radtke J, Vinsensia M, Lehnert W, et al. F-18 labelled PSMA-1007: Biodistribution, radiation dosimetry and histopathological validation of tumor lesions in prostate cancer patients. Eur J Nucl Med Mol Imaging, 2017; 44(4): 678–688.
- Budäus L, Leyh-Bannurah SR, Salomon G, Michl U, Heinzer H, Huland H, et al. Initial Experience of 68Ga-PSMA PET/CT Imaging in High-risk Prostate Cancer Patients Prior to Radical Prostatectomy. Eur Urol, 2016; 69(3): 393–396.
- Lütje S, Franssen GM, Herrmann K, Boerman OC, Rijpkema M, Gotthardt M, et al. In Vitro and In Vivo Characterization of an 18F-AlF-Labeled PSMA Ligand for Imaging of PSMA-Expressing Xenografts. J Nucl Med, 2019; 60(7): 1017-1022.
- Ioppolo JA, Nezich RA, Richardson KL, Morandeau L, Leedman PJ, Price RI. Direct in vivo comparison of [18F]PSMA-1007 with [68Ga]Ga-PSMA-11 and [18F]AlF-PSMA-11 in mice bearing PSMA-expressing xenografts. Appl Radiat Isot, 2020; 161: 109164.
- Giesel FL, Will L, Lawal I, Lengana T, Kratochwil C, Vorster M, et al. Intraindividual Comparison of 18F-PSMA-1007 and 18F-DCFPyL PET/CT in the Prospective Evaluation of Patients with Newly Diagnosed Prostate Carcinoma: A Pilot Study. J Nucl Med, 2018; 59(7): 1076-1080. doi: 10.2967/jnumed.117.204669.
- Rahbar K, Afshar-Oromieh A, Seifert R, Wagner S, Schäfers M, Bögemann M, et al. Diagnostic performance of 18F-PSMA-1007 PET/CT in patients with biochemical recurrent prostate cancer. Eur J Nucl Med Mol Imaging, 2018; 45(12): 2055-2061. doi: 10.1007/s00259-018-4089-x.
- Artigas C, Alexiou J, Garcia C, Wimana Z, Otte FX, Gil T, et al. Paget bone disease demonstrated on 68Ga-PSMA ligand PET/CT. Eur J Nucl Med Mol Imaging, 2016; 43(1): 195–196.
- Krohn T, Verburg FA, Pufe T, Neuhuber W, Vogg A, Heinzel A, et al. [68Ga]PSMA-HBED uptake mimicking lymph node metastasis in coeliac ganglia: an important pitfall in clinical practice. Eur J Nucl Med Mol Imaging, 2015; 42(2): 210–214.
- Hirmas N, Al-Ibraheem A, Herrmann K, Alsharif A, Muhsin H, Khader J, et al. [68Ga]PSMA PET/CT Improves Initial Staging and Management Plan of Patients with High-Risk Prostate Cancer. Mol Imaging Biol, 2019; 21(3): 574–581.

