Differentiated Thyroid Cancer in Children: A Case Report and Incidentally Visualization of The Thymus on Whole Body Iodine Scan
Gerardo Gabriel dos Santos Loureiro*, Eduardo Lischinsky and Omar Alonso Nuñez
Nuclear Medicine and Molecular Imaging Centre, Hospital de Clínicas, Universidad de la República, Avenida Italia s/n; Montevideo 11600, Uruguay
Received Date: 31/05/2025; Published Date: 01/07/2025
*Corresponding author: Gerardo Gabriel dos Santos Loureiro, MD, PhD, Nuclear Medicine and Molecular Imaging Centre, Hospital de Clínicas, Universidad de la República, Avenida Italia s/n; Montevideo 11600, Uruguay
Abstract
Differentiated thyroid cancer (DTC) is the most common type of thyroid malignancy in children and presents distinct diagnostic and therapeutic challenges due to its higher metastatic potential compared to adults.
We report the case of a 10-year-old boy diagnosed with papillary thyroid carcinoma with a follicular pattern. Initial imaging and biopsy revealed a solid thyroid nodule, and subsequent thyroidectomy confirmed malignancy with vascular and lymphatic invasion. Post-operative radioactive iodine therapy and whole-body scintigraphy suggested pulmonary metastasis. Unexpected intense mediastinal uptake on follow-up imaging was identified as physiological thymic activity, highlighting a rare but important potential false-positive finding in whole-body scans.
Pediatric DTC often presents with high-risk features including metastasis but responds well to treatment. Recognition of physiological thymic uptake is essential to avoid misinterpretation as metastatic disease on post-therapeutic scans.
Keywords: Differentiated thyroid cancer, pediatric, radioiodine, thymus visualization
Case Presentation
Differentiated thyroid cancer (DTC) is the most common pathology in children that usually presents with thyroid nodules with a considerable risk of malignancy [1].
We present the case of a 10-year-old boy with an incidental enlargement of the neck (10/2007).
Ultrasound: solid nodule in the right lobe of the thyroid. Fine needle aspiration biopsy (3/2007): a predominant parenchymal nodule, with marked morphological abnormalities, Hurtle and histiocyte cells.
Thyroid Scintigraphy (3/12/07) revealed an area of hypofunction in the lower pole of the right lobe (palpable nodule) (Figure 1A).
He underwent thyroidectomy (26/12/2007).
Pathologic examination (27.12.07) revealed papillary thyroid carcinoma with follicular pattern, vascular and perineural infiltration, extraglandular extension and lymph-node metastasis.
He receibed a therapeutic dose of 100 mCi of radioactive iodine on 18.2.08.
Post-operative thyroid scintigraphy showed intense uptake in thyroid remnant and in thorax in a diffuse pattern suggesting lung metastasis (Figure 1B).
Although lung metastasis from differentiated thyroid cancer in children is estimated at 25% (3–4 times higher than in adults), they may respond to radioactive iodine therapy and overall survival is excellent [2].
Chest X-ray: bilateral miliary seeding. CT: disseminated pulmonary nodules. Respiratory function: normal. Subsequent WBS (08/2008) showed residual thyroid gland. (Figure 1C) leading to a second therapeutic dose (130 mCi; 07/09/2009).
On posttreatment scintigraphy intense upper mediastinal uptake is noted, corresponding to probable thymic tissue. (Figure 2A) which is an uncommon cause of false-positive that might be considered as lung or mediastinal nodes metastases [3].
Subsequent serial negative (last Tg 1.72 ng/ml) (Figure 2B).
We presented a pediatric patient with a high risk of persistence/recurrence and physiological thymus uptake: a potential cause of false-positive WBS. DTC has a good prognosis in metastatic pediatric population. An individualized risk-based approach is mandatory for adequate therapy.
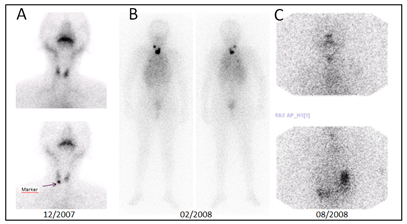
Figure 1
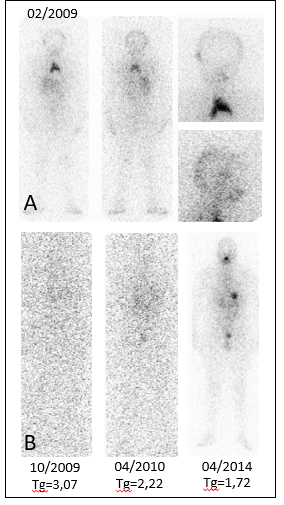
Figure 2
Conclusion
This case underscores the importance of a careful, individualized, risk-based approach in managing pediatric differentiated thyroid cancer. Although metastatic presentations are more common in children, prognosis remains excellent. Awareness of physiological thymic uptake is crucial to prevent false-positive interpretations on whole-body iodine scans and to guide appropriate management decisions.
Compliance with Ethical Standards:
The procedure performed was in accordance with the ethical standards of the institutional research committee of CUDIM and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent: Informed consent was obtained from the patient included in the study.
No conflict-of-interest exists.
The manuscript has been read and approved by all the authors. The requirements for authorship have been met. Each author believes that the manuscript represents honest work.
References
- Lamartina L, Leboulleux S, Schlumberger M. Thyroid cancer incidence in children and adolescents. Lancet Diabetes Endocrinol, 2021; 9(3): 128-129.
- Chesover AD, Vali R, Hemmati SH, Wasserman JD. Lung Metastasis in Children with Differentiated Thyroid Cancer: Factors Associated with Diagnosis and Outcomes of Therapy. Thyroid, 2021; 31(1): 50-60.
- Mello ME, Flamini RC, Corbo R, et al. Radioiodine concentration by the thymus in differentiated thyroid carcinoma: report of five cases. Arq Bras Endocrinol Metabol, 2009; 53: 874–879.

