Tracheal Injuries in Children
Badie Douqchi1,*, Doaae El Ouaddane2, Omar Alaoui Mhammedi1, Amine Elmouhib1, Mohammed El Aissaouy1, Houassam Bkiyar1,3 and Brahim Housni1,3
1Department of Anesthesia and Reanimation, Mohammed VI University Hospital, Morocco
2Department of Thoracic surgery , Mohammed VI University Hospital, Morocco
3Faculty of Medicine and Pharmacy, Mohammed Ist University, Morocco
Received Date: 26/05/2025; Published Date: 26/06/2025
*Corresponding author: Badie Douqchi, Department of Anesthesia and Reanimation, Mohammed VI University Hospital, Oujda, Morocco
Abstract
Tracheal trauma is rare and often serious, particularly in children. While management is standardized in adults, allowing for rapid decision-making, the role of different examinations is less clear in pediatrics.
We describe the case of a 4-year-old child whose CT scan allowed us to decide on the course of action without prior bronchial endoscopy.
In light of this clinical case and a review of the literature, we propose a review of this condition and its management.
Introduction
Tracheobronchial trauma related to chest compression injuries is a rare condition with a prevalence of more than 1% of the compression trauma population [1]. Their incidence is even lower in children, the main cause of which is public transport accidents [2,3]. Rapid diagnosis and management should be a priority, as mortality can reach 30%, half of which occurs within the first hour [4].
A direct relationship has been established between the speed of treatment and morbidity, even in the long term, regardless of the quality of this treatment [3]. We describe here the case of a child for whom conservative treatment was decided upon upon diagnosis of tracheal injury.
Case Report
It is a 4 -year-old child, with no particular medical history, suffered a direct anterior cervical trauma from the handlebars of his bicycle. He was quickly referred to the emergency department for diffuse facial edema associated with inspiratory pain.
At the admission, his hemodynamic parameters were stable. He presented with painful dyspnea in both phases but saturation on room air: 90%, 99% under 2L O2. There was a main contusion in the anterior cervical region associated with diffuse subcutaneous emphysema of the trunk and cephalic extremity (Figure 1). Pulmonary auscultation was otherwise clear and symmetrical. The remainder of the examination was unremarkable. Due to the child's general stability, an emergency cervicothoracic CT scan was performed (Figure 2).
CT scanner revealed a tracheal rupture of the posterior edge of the cervicothoracic trachea at the level of C7-T1, approximately 4 mm in length, complicated by a pneumomediastinum without involvement of the mediastinal organs, as well as significant subcutaneous emphysema. low-volume both sides pneumothorax (Figure 3). There was no pulmonary parenchymal abnormality, nor at the level of the cervical spine or rib cage.
Conservative management was decided upon and the child was hospitalized in intensive care for prophylactic antibiotic therapy (amoxicillin-clavulanic acid-gentamicin), with dietary withdrawal and monitoring of the clinical condition. In case of worsening, a fibroscopy was to be performed, followed by tracheal intubation distal to the lesion. The parents were informed that if this failed, a tracheotomy would be performed distal to the lesion to allow the trachea to heal.
The clinical evoution was favorable, with spontaneous respiratory function remaining stable, without oxygen dependence. Seven days after the injury, a follow-up imaging study showed a marked improvement in the pneumomediastinum and subcutaneous emphysema, with the development of a low-volume right pneumothorax. The tracheal defect had closed, leaving a parietal irregularity.
The follow-up was uneventful, with the emphysema gradually diminishing. After 25 days of monitoring, the completely asymptomatic child was able to return home. Several weeks of clinical and radiographic follow-up with rest at home revealed no complications. Three months after the trauma, a bronchial fibroscopy showed a normal trachea, not scarred and without variation in caliber.
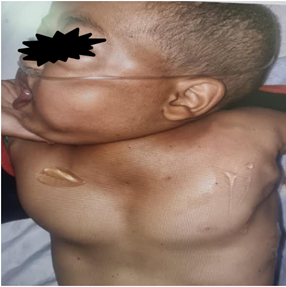
Figure 1: Image of our patient with diffuse subcutaneous emphysema of the trunk and cephalic extremity.
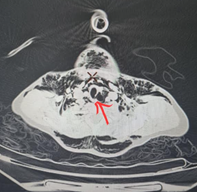
Figure 2: CT image showing tracheal rupture of the posterior edge of the cervicothoracic trachea at the level of C7-T1, approximately 4 mm in length, complicated by a pneumomediastinum.
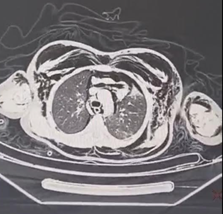
Figure 3: CT scanner shows a pneumomediastinum without involvement of the mediastinal organs, as well as significant subcutaneous emphysema. Low-volume both sides pneumothorax.
Discussion
Tracheal trauma is secondary to compression injuries, penetrating wounds, or of iatrogenic origin (traumatic intubation) [3]. These are serious conditions that can lead to severe respiratory failure and hemodynamic instability. Diagnosis can sometimes be difficult given the paucisymptomatic presentation of some patients with small lesions [5,6].
The specific anatomy of children helps reduce the incidence of this type of trauma: their relatively wide cephalic extremity and rib cage protect a relatively short neck. In addition, the mobility and compressibility of the tracheal cartilages further reduce the risk of injury [3]. However, once the trachea is injured, it is important to provide prompt treatment. A small larynx, larger arytenoids, and a prominent epiglottis contribute to a narrowing of the laryngeal lumen and complicate ventilation [7]. The main mechanism of tracheal injury in children remains external compression directly applied to the anterior aspect of the neck. Falls on playgrounds and bicycle accidents are the most common causes: at the moment of impact, the child's neck is hyperextended and the exposed larynx hits the handlebars (Padded Dash Syndrome) [8]. The cartilage then compresses, and the transmitted force is transmitted to the posterior tracheal wall, which compresses the cervical spine. This phenomenon mainly results in horizontal or irregular linear lesions of the posterior wall. In contrast, iatrogenic tracheal injuries result in longitudinal lesions of the posterior wall [9]. Most of these lesions are located 2.5 cm above the carina or at the level of the right main bronchus [10].
The most common clinical signs are subcutaneous emphysema, respiratory distress, and hemoptysis. Some patients may also present with pneumothorax or pneumomediastinum [1,3–6,9]. However, it is important to keep in mind that many patients may present with few symptoms. For any patient suspected of tracheal trauma, the priority remains to ensure good ventilation. This may involve evacuation of a pneumothorax, resuscitation, or endotracheal intubation if the patient is unstable. A complete injury assessment must then be performed: this includes a chest X-ray to look for a pneumothorax, pneumomediastinum, or to assess subcutaneous emphysema; an interruption of the tracheal air column or atelectasis are highly suggestive. This assessment must be combined with X-rays of the cervical spine to look for fractures of the spine or rib cage [3]. The role of cervicothoracic CT scan varies according to the authors. It may delay treatment and should therefore not be preferred when the patient is unstable [1,3,5]. However, it is very useful in stable patients with abnormalities detected on the chest X-ray. It allows for a complete assessment of the spine and provides a precise lesion (tracheal injury) and peri-lesion cervicothoracic assessment (esophageal, pulmonary, aortic involvement) [4,9].
The gold standard for diagnosing tracheobronchial trauma remains bronchial endoscopy. It should ideally be performed by a pulmonologist or thoracic surgeon in the operating room [1,3–5,9]. It allows for a precise lesion assessment, the determination of a possible surgical indication, and the provision of visually controlled endotracheal intubation, excluding the lesion if necessary. However, given the quality of the images and the precision of the reconstructions of the tracheobronchial tree currently available in the recent scanners, the role of this invasive examination can, in our opinion, be debated. Furthermore, conservative management should be considered as a matter of principle for these injuries, particularly in pediatrics and in the absence of signs of severity.
Management of tracheal injuries after stabilization of the patient is dictated by the patient's clinical condition and the characteristics of the injury. In case of respiratory and hemodynamic stability, conservative treatment based on systemic corticosteroids, proton pump inhibitors and possibly antibiotic prophylaxis can be undertaken [9]. In cases of respiratory instability with preserved hemodynamics, or in cases of severe tracheal lesions (circular lesion involving the entire tracheal thickness, > 2 cm, involvement of the pericarial region), reconstructive surgery is indicated. Finally, in the event of hemodynamic and respiratory instability, surgery not being possible, extracorporeal circulation techniques (extracorporeal membrane oxygenation [ECMO]) can be used [5]. In our case, the severity of which was moderate, with preserved respiratory function, a chest CT scan appeared to be the first-line examination, avoiding all the potential complications of an emergency bronchial endoscopy. It also did not seem necessary to perform a bronchial endoscopy immediately afterward, since the lesions had been clearly visualized on the CT scan and were deemed minimal, and respiratory function was always preserved.
Conclusion
Tracheal trauma is a serious condition requiring a comprehensive initial assessment. Conservative treatment plays a significant role in children; it is reliable and avoids invasive procedures that can potentially cause complications, while ensuring a good long-term functional prognosis.
References
- Roux P, Fisher RM. Chest injuries in children: an analysis of 100 cases of blunt chest trauma from motor vehicle accidents. J Pediatr Surg, 1992; 5: 551–555.
- Verstraeten AF, Westermann CJJ, Knaepen J, et al. Les le´sions tracheobronchiques lors des traumatismes fermes du thorax. Rev Mal Respir, 1992; 9: 623–628.
- Ducasseé JLRJ, Caussade D, Villacèque E, et al. Rupture trachéale au décours d’un traumatisme thoracique : intérêt diagnostique de la fibroscopie bronchique et de la tomodensitométrie hélicoïdale. Réanimation urgences, 1999; 8: 697–700.
- Ballouhey Q, Fesseau R, Benouaich V, et al. Benefits of extracorporeal membrane oxygenation for major blunt tracheobronchial trauma in the paediatric age group. Eur J Cardiothorac Surg, 2013; 43: 864–865.
- Wood JW, Thornton B, Brown CS, et al. Traumatic tracheal injury in children: a case series supporting conservative management. Int J Pediatr Otorhinolaryngol, 2015; 79: 716–720.
- Rossbach MM, Johnson SB, Gomez MA, et al. Management of major tracheobronchial injuries: a 28-year experience. Ann Thorac Surg, 1998; 65: 182–186.
- Fette A, Hollwarth ME. Tracheobronchial injuries in childhood: review of two cases. J Pediatr Surg, 2001; 36: 521–523.
- Heldenberg E, Vishne TH, Pley M, et al. Major bronchial trauma in the pediatric age group. World J Surg, 2005; 29: 149–154.
- Boubiaa S, Fouraijib K, Elkaric A, Sibaib H, Chlilekc M, Ridaia M. Tracheobronchial rupture in childhood Archives de Pédiatrie, 2010; 17: 1059-1061.
- Myer 3rd CM, Orobello P, Cotton RT, et al. Blunt laryngeal trauma in children. Laryngoscope, 1987; 97: 1043–1048.

